
1. Reversing aging in mice
Dutch researchers have found a way to reverse certain aspects of aging in mice. Researchers at the Erasmus University Medical Center in Rotterdam achieved this by giving the mice a peptide that prevents two proteins from binding.
As a result, the mice became fitter and more alert, their coats became fuller, and their organ functions improved. This was achieved by giving the mice proxofim, a substance that was created by the researchers themselves, which disrupts the binding of the FOXO4 and P53 proteins.
Unlike existing substances that intervene with aging, proxofim was found to have no adverse side effects on the health of the mice. This is because it can deal with “senescent” cells that are significant contributors to the aging process.

Senescent cells are cells that cease to divide, but are not really dead. Their metabolism actually continues to function, resulting in all kinds of proteins being secreted. These proteins have a negative effect on the mice, causing more rapid aging of tissue and diminished organ function.
Proxofim actually kills these senescent cells and stimulates cells that surround them to create new tissues. What’s more is that since proxofim is a peptide, it can easily penetrate into cells. After just three weeks of being administered proxofim, the mice were observed to be up to three times as active on their running wheels, as well as exhibiting increased organ function and a thickening of their coats.
The researchers have stated that they wish to continue investigating the safety and efficacy of proxofim further prior to starting human trials in a year or two. These trials will take place using patients that have been diagnosed with aggressive forms of cancer, and then expanded to individuals suffering from geriatric ailments.
This study was published in the leading scientific journal, Cell.
2. Two-way communication between artificial limbs and the brain
Neuroscientists at the University of Geneva have found a way to create an artificial neural signal that allows individuals who use neural prostheses to feel sensations similar to those that a fully-able bodied person would feel through their natural limbs.
This incredible breakthrough has achieved what scientists have been trying to achieve for the best part of 40 years, with limited success. Previous methods have employed the use of electrodes, but the Swiss neuroscientists decided to shun that approach and try something else.
What they came up with was transmission of the missing sensation from the neural prosthesis back to the brain through the stimulation of the neural cortex. What they found stunned them – not only was it possible for an artificial sensation of neuroprosthetic movements to be created, but the underlying learning process occurred very rapidly as well.

This was achieved by using optical techniques for imaging and stimulating brain activity, specifically a method called two-photon microscopy. The researchers wanted to see if mice could learn to control a neural prosthesis by relying solely on an artificial sensory feedback signal. When they activated a specific neuron in their brains, the one chosen for neuroprosthetic control, they simultaneously applied stimulation proportional to the activity to the sensory cortex using blue light.
These neurons were found to be photosensitive to light, meaning that they could be activated by a series of optical flashes and allowed the researchers to integrate the required artificial sensory feedback signal.
In other words, the researchers managed to create a brain-machine interface (the brain and the neural prosthesis communicating with one another) that functions bi-directionally. They hope that this will allow the precise displacement of robotic arms, allowing people to feel the sensation of touch using their neural prostheses, as well as allowing them to perceive the necessary force required to pick up and hold objects.
This study was published in the leading scientific journal, Neuron.
3. Nanoelectric thread brain probes
Researchers at the University of Texas in Austin have developed new nanoelectric brain probes that are more than 1,000 times more flexible than existing neural probes, which are hoped to be able to increase the ability of medical practitioners to record and track neural activity for extended periods of time.
Existing neural probes often cause problems due to their size and mechanical stiffness. They often cause damage around the tissue they encompass, and they also often provide unreliable recordings. Another problem is that it’s difficult for them to track individual neurons for more than a few days.
In contrast, the UT Austin research team’s electrodes are flexible enough to comply with micro-scale tissue movements and still remain in place. Due to their tiny size, the electrodes (probes) are much less likely to displace brain tissue, resulting in a more stable brain interface and much more accurate readings over longer periods of time.
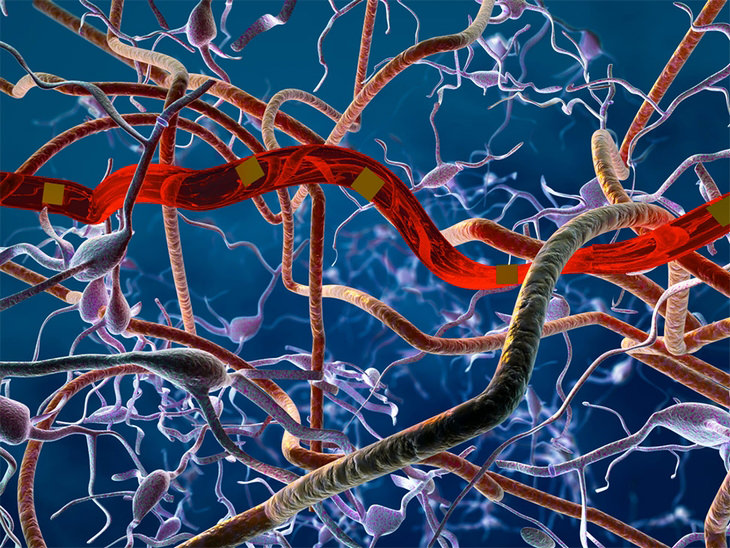
The new brain probes are so small that they are as little as 10 microns long, and less than 1 micron wide. Just as a point of reference, the average human hair is between 40 and 50 microns wide. They’re even smaller than neurons and capillaries, and are widely believed to be the smallest neural probes ever developed.
The biggest plus of this new technology is that interference with biological systems is kept to a minimum. When the probes were tested on mice, they were found to prevent the agitation of glial cells thanks to their flexibility and size. This means that they avert a normal biological reaction that normally occurs when a foreign body is implanted.
Researchers would like to continue experimenting on animals for a while, but it’s hoped that clinical trials on humans could start in the near future. Human applications that are envisaged include use in high-performance prostheses, as well as for tracking progression of neurodegenerative and neurovascular diseases such as strokes, Parkinson’s and Alzheimer’s.
This study was published in the leading scientific journal, Science Advances.
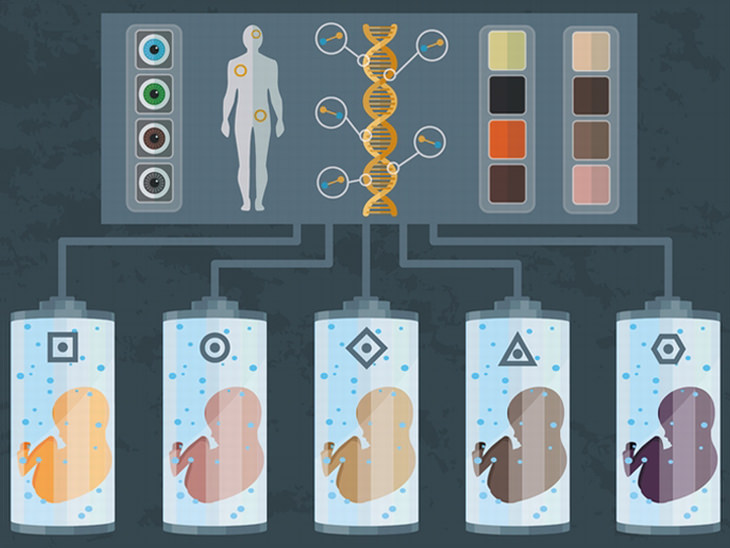
4. US government-approved gene editing for human embryos
This one isn’t a medical breakthrough as such, because gene editing has been around for a while – it’s more of a breakthrough in the attitude about the gene editing of human embryos. The US National Academy of Sciences and the National Academy of Medicine have given their backing for gene editing of human embryos to go ahead, albeit under highly stringent conditions.
The clinical trials that are currently permitted are only allowed for treating or preventing diseases or disabilities at the time. This has become possible due to the emergence of powerful, precise and less costly genome editing tools, which in turn led to an explosion of new research opportunities and potential clinical applications.
Heritable and non-heritable health problems could be addressed as a result of successful clinical trials. As you can imagine, the future potential for vastly diminishing, if not entirely eradicating pervasive human health issues, is huge.
Due to the risky nature of gene editing, the NAS and NAM have appointed an oversight committee consisting of international experts to examine the scientific, ethical and governance issues related to gene editing.
There are numerous ethical issues surrounding this latest approval, such as whether it can be ensured that this type of technology is only used for the right things, as opposed to things that are viewed as being unethical.
Although this kind of scenario was seen as science fiction just a few years ago, the fact that technology has advanced so much has left us all facing serious and urgent social justice questions. For instance, the wealthy and privileged are on the verge of being able to use these high-tech procedures to create children with biological advantages. If this technology is left to develop and advance unbridled by the proper constraints, a disastrous scenario of social inequality could arise – “superior” gene-edited individuals, versus those who have parents that did not have the economic means to ensure that all the possible hereditary problems were eradicated prior to their birth.
The regulatory approval announcement was published in Human Genome Editing: Science, Ethics and Governance..
5. A machine that can 3D print human skin
Scientists at the Universidad Carlos III De Madrid’s Center for Energy, Environmental and Technological Research have developed a prototype 3D bioprinter that is capable of printing fully functional human skin.
It’s hoped that the skin will be used for transplanting to patients, as well as for researching and testing cosmetic, chemical and pharmaceutical products. It replicates the natural structure of human skin, with an external layer (the epidermis, which protects us from the external environment) and a thicker, deeper layer (the dermis).
The dermis layer consists of fibroblasts that produce collagen, the protein that gives the skin elasticity and its mechanical strength to move and stretch. In addition, there’s another key component at play in order to create the skin. Think of bioinks as the biological equivalent of printer cartridges and colored inks. These are mixed in precise conditions so that the cells they contain don’t deteriorate.

In fact, knowing how to mix the various biological components that go into creating the skin is crucial to the entire process. This mixing is controlled by a computer, which in turn deposits the mixture on a print bed in a precise and orderly fashion.
Currently, the scientists have two different ways of making these tissues. The first is for producing allogeneic skin from a stock of cells on a large scale for industrial processes, and the second is autologous skin, which is created using a patient’s own cells and is designed for therapeutic applications, such as for the treatment of severe burns.
Some of the benefits of this new 3D-printed human skin include standardized, automated generation, reduced costs when compared to manual production, and the possibility of cosmetic and consumer chemical product testing that cannot be conducted on animals.
This study was published in the leading scientific journal, Biofabrication.
Bonus - Watch the lead developer of the 3D bioprinter talk about it in his own words:
Content and image source: Future Timeline
Related Articles:
The 10 Strangest Medical Cases From 2017
7 Medical Mysteries That Continue To Baffle Doctors
The 10 Most Bizarre Medical Cases of 2019