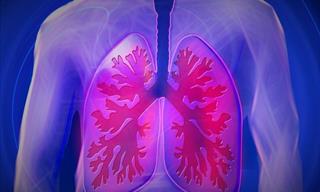
The top cause of COPD is smoking, while long-term exposure to chemical irritants can also cause it. There’s no cure for COPD, which is diagnosed via blood tests, imaging tests, and lung function tests, but there is a treatment that can help to ease the symptoms and improve quality of life. Such treatment includes oxygen therapy, medication, and surgery.
Around 24 million people in the United States suffer from COPD – as many as half are oblivious to the fact that they have it. Find out more about this debilitating illness below:
What Are the Symptoms?
Early symptoms include:
• Occasional shortness of breath
• A mild but recurrent cough
• Needing to clear your throat a lot, especially first thing in the morning
As your lungs become more damaged, you might experience:
• Shortness of breath, even after mild exercise such as walking up some stairs
• Wheezing or noisy breathing
• Chest tightness
• Chronic cough, with/without mucus
• Frequent colds, flu or other respiratory infections
• A lack of energy
In the later stages of COPD, symptoms might also include:
• Swelling of the ankles, feet, or legs
• Weight loss
• Fatigue
Immediate medical care should be sought if:
• You have bluish or gray fingernails or lips (this indicates low oxygen levels in your blood
• You have difficulty catching your breath or cannot talk
• You feel confused and faint
• Your heart is racing
What Causes COPD?

As briefly mentioned above, the single biggest cause of COPD is cigarette smoking. In fact, about 90% of people who have COPD are smokers or former smokers. Among smokers, around 20-30% develop COPD, while many others develop lung conditions or have reduced lung function.
The majority of people with COPD are over 40 years old and have some history of smoking. The longer you smoke, the greater your risk of developing COPD. Long-term exposure to air pollution and inhaling dust can also cause COPD.
There might also be a genetic predisposition to developing COPD as well. Up to 5% of people with this illness have a deficiency in a protein known as alpha-1-antitrypsin. This deficiency causes the lungs to deteriorate and can also affect the liver.
Diagnosing COPD
There’s no single test to diagnose COPD. Diagnosis is based on symptoms, a physical exam, and test results.
When you visit the doctor, be sure to mention all of your symptoms. Tell your doctor if:
• You’re a smoker or have smoked in the past
• You’re exposed to lung irritants at work
• You’re exposed to a lot of secondhand smoke
• There’s a family history of COPD
• You have asthma or other respiratory conditions
• You take over-the-counter or prescription medications
During the physical exam, your doctor will use a stethoscope to listen to your lungs as you breathe. Based on what he hears, your doctor might order some of these tests to get a more complete picture:

• A spirometry – This is a noninvasive test to assess lung function. During the test, you’ll take a deep breath and then blow into the tube connected to the spirometer.
• Imaging tests – These include a chest X-ray or a CT scan. These images can provide a detailed look at your lungs, heart, and blood vessels.
• An arterial blood gas test – this involves taking a blood sample from an artery to measure the oxygen levels in the blood.
Treatment for COPD
Treatment can help to ease the symptoms, prevent complications, and slow the disease down.
Medication
Bronchodilators are medications that help to relax the muscles of the airways so that you can breathe easier. They’re usually taken using an inhaler. Glucocorticosteroids can be added to decrease inflammation in the airways.
To lower your risk of other respiratory infections, ask your doctor whether you should get a yearly flu shot, pneumococcal vaccine, and a tetanus booster that includes protection from whooping cough.
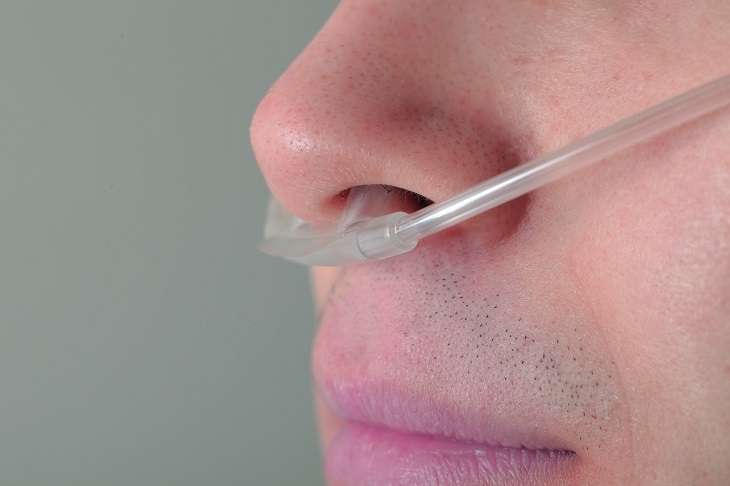
Oxygen Therapy
If your blood oxygen levels are too low, you can receive oxygen through a mask or nasal prongs to help you breathe better. A portable unit can make it easier to get around.
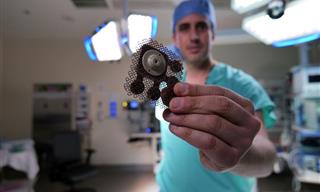
Surgery
Surgery is only used when the COPD is severe and all other treatments have failed, which is more likely the case if you have emphysema. One type of surgery is a bullectomy, which is when surgeons remove large sir sac (bullae) from your lungs. Another is lung volume reduction surgery, which removes damaged lung tissue.
In very extreme cases, a lung transplant is also an option.
Lifestyle Changes
Certain lifestyle changes might also help to alleviate your symptoms or provide some relief. These include:
• Quitting smoking. Your doctor can recommend appropriate products or support services.
• Whenever possible, avoid secondhand smoke and chemical fumes.
• Get the nutrition that your body needs. Work with your local dietitian or doctor to create a healthy eating plan.
• Talk to your doctor about how much exercise is safe for you.
Diet Recommendations for People with COPD

There’s no particular diet for COPD, but a healthy diet is important for overall health. The stronger you are, the more likely it is that you’ll be able to prevent complications and other health problems.
Choose a variety of nutritious foods from these groups:
• Fruits
• Vegetables
• Grains
• Protein
• Dairy
Drink plenty of fluids too. Drinking six-eight glasses of non-caffeinated liquids every day can help to keep mucus on the thin side. This will make the mucus easier to clear out. You need to limit caffeinated beverages as they can interfere with medications and increase water loss.
Your weight is important as it takes more energy to breathe when you have COPD, so you might need to take in more calories. If you’re overweight, your lungs and heart might have to work harder. If you happen to be underweight or frail, even basic body maintenance can become difficult. Overall, having COPD weakens your immune system and decreases your ability to fight off infection.
A full stomach makes it harder for your lungs to expand, leaving you short of breath. If this happens, try the following remedies:
• Clear your airways about an hour before a meal.
• Swap three meals a day for five or six smaller ones.
• Save fluids until the end so you feel less full during the meal.
What Are the Stages of COPD?
One measure of COPD disease is by stage. The stages are as follows:
Stage 0 – At risk: Symptoms include coughing and noticeable mucus. You don’t actually have COPD at this stage, so treatment isn’t necessarily needed. However, you should heed the warning. If you smoke, stop it. It would also be wise to reassess your diet and exercise routines to improve your overall health. Once you do have COPD, it’s not reversible or curable.
Stage 1 – Mild: At this stage, some people still don’t notice the symptoms, which might include a chronic cough and increased mucus production. If you visit a doctor at this point, chances are you’ll start using a bronchodilator as needed.
Stage 2 – Moderate: Symptoms will become more noticeable. In addition to a cough and mucus, you might start to experience shortness of breath. You might need a long-acting bronchodilator.
Stage 3 – Severe: Symptoms become more frequent and you might have occasional flare-ups of severe symptoms. You may find it difficult to function normally. Your doctor might recommend corticosteroids or oxygen therapy.
Stage 4 – Very Severe: The symptoms are progressing and it’s harder to complete everyday tasks. Flare-ups can be life-threatening. You might be a candidate for surgical treatment.
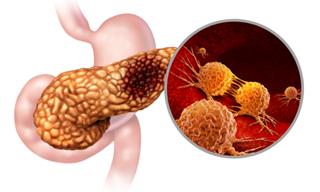
Is There a Connection between COPD and Lung Cancer?
All over the world, COPD and lung cancer are major health problems. These two diseases are linked in a number of ways.
For example, COPD and lung cancer have several common risk factors. Smoking is the number one risk factor for both diseases. They’re both more likely if you breathe in secondhand smoke, or are exposed to chemicals or other fumes in the workplace.
There might be a genetic predisposition to developing both diseases. Furthermore, the risk of developing either condition increases with age.
Between 40 and 70% of people with lung cancer also have COPD. Therefore, a 2009 study concluded that COPD is, indeed, a risk factor for lung cancer.
What’s the Outlook for People with COPD?
COPD tends to progress slowly, so you might not even know you have it in the early stages. Once you have been diagnosed, you’ll need to start seeing your doctor on a regular basis. You’ll also have to take steps to manage your illness and make the appropriate changes to your daily life.
The early symptoms can be managed, and certain lifestyle choices can help you to maintain a good quality of life for some time.
As your disease progresses, symptoms can become increasingly limiting. In the severe stages of COPD, you might not be able to care for yourself with assistance. You’re also at an increased risk of developing other respiratory infections, heart problems, and lung cancer. You might also be at risk of depression.
Those with COPD tend to have a lower life expectancy, though the outlook varies considerably from person to person. People with COPD who have never smoked may have a modest reduction in life expectancy, while those who have smoked or still do are likely to have a larger reduction.
Besides smoking, your outlook depends on how well you respond to treatment and whether you can avoid serious complications. Your doctor will be able to evaluate your overall health and give you an idea of what to expect.
 Go to BabaMail
Go to BabaMail