A recent study has unveiled a potential breakthrough in addressing glioblastoma, the most lethal brain cancer type.
Treating brain tumors presents unique challenges primarily because the blood-brain barrier, a protective mechanism regulating the passage of substances from the bloodstream to the brain, hinders the effectiveness of most chemotherapy medications.
Northwestern Medicine scientists recently employed an implanted ultrasound device within the brain to temporarily create an opening in the blood-brain barrier. This breakthrough enabled the delivery of chemotherapy drugs to the brain through intravenous injection.
See Also: Common Anti-Diarrhea Drug Found to Kill Brain Cancer Cells
Dr. Jason Salsamendi, the lead interventional radiologist at the City of Hope Orange County Lennar Foundation Cancer Center in California, expressed his optimism about the findings, stating, "The discovery that a novel technology can safely and effectively facilitate the opening of the blood-brain barrier to administer chemotherapy represents a potentially groundbreaking advancement in brain cancer research and treatment." This comment was made in an interview with Medical News Today.
The study, published in the journal Lancet Oncology, reports that a procedure lasting four minutes was performed on patients while they were awake. This procedure was repeated every few weeks for a total of six sessions spanning a four-month period. The study revealed a significant increase in the concentration of chemotherapy drugs within the brain, ranging from nearly four to sixfold.
The significance of the latest brain cancer treatment
The research focused on the use of paclitaxel and carboplatin, which are powerful chemotherapy medications typically unsuitable for treating glioblastoma.
Temozolomide, the primary chemotherapy drug presently employed against glioblastoma, can cross the blood-brain barrier, but it is relatively ineffective.
As mentioned earlier, the blood-brain barrier is a tiny structure that acts as a shield, preventing the majority of drugs in the bloodstream from reaching the brain. This limitation severely restricts the range of drugs available for the treatment of brain-related diseases. For instance, patients with brain cancer cannot benefit from many medications that effectively treat cancer in other parts of the body because these drugs are unable to cross the blood-brain barrier. To successfully repurpose drugs for treating brain diseases, including cancer, it is crucial to find a way to deliver them to the brain.
See Also: Knowing the Signs of a Brain Tumor Can Save Your Life...
Previous studies attempted to address this challenge by directly injecting paclitaxel into the brains of patients with brain tumors. Although these studies showed promising indications of effectiveness, the direct injection method was accompanied by adverse effects such as brain irritation and meningitis, explains Dr. Adam Sonabend, an associate professor of neurological surgery at Northwestern University Feinberg School of Medicine and a neurosurgeon at Northwestern Medicine.
The researchers in the recent study discovered that the blood-brain barrier, once forcibly opened, quickly sealed up again, usually within 30 to 60 minutes.
Salsamendi says it is important to understand the duration for which the blood-brain barrier remains open because the longer it stays open, the higher the chance of harmful substances entering the brain. Accurate understanding of how long the barrier remains open is important for effective treatment planning and mitigating possible dangers.
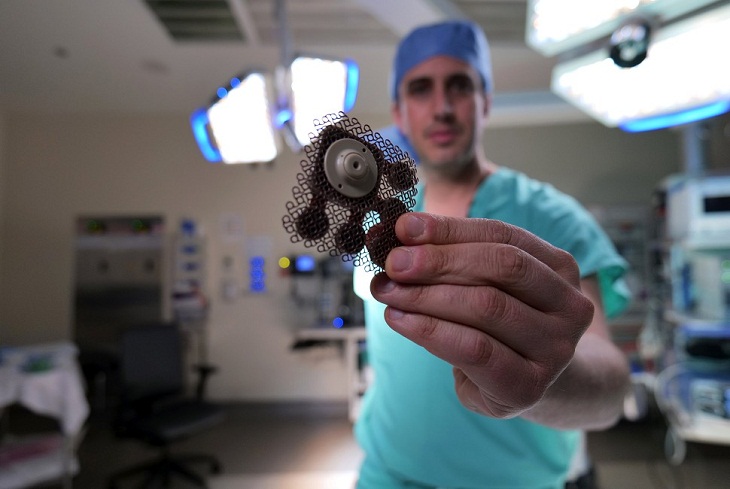
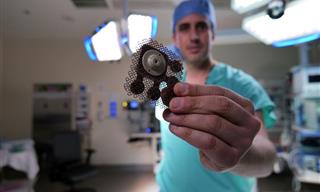
The groundbreaking ultrasound device opens the blood-brain barrier, delivering chemotherapy to vital brain regions. (Image Credit: Northwestern University)
Developed by Carthera, a biotechnology company based in France, the ultrasound device operates by employing a stream of microbubbles to unlock the blood-brain barrier.
See Also: Cancer Breakthrough: Blood Test That Detects Five Cancers
By creating a sizable gap in the barrier, these ultrasound devices are intended to significantly enhance the effectiveness of chemotherapy when it is administered to an expanded region of the brain after surgical tumor removal, emphasizing their pivotal role.
At present, the same group of researchers is executing clinical studies to evaluate whether the transfer of paclitaxel and carboplatin through the blood-brain barrier has the potential to extend the lifespan of individuals afflicted with recurrent glioblastoma tumors. The combined use of these two drugs has been proven effective in addressing other types of cancer.
 Go to BabaMail
Go to BabaMail