
These are difficult times. The novel coronavirus pandemic has gripped the entire world in its tentacles and news of misery and gloom keep following us every day from each corner of the globe. So, is there no hope in sight?
Even as we write this, about 300 separate trials into different drugs and experimental therapies have been launched in the absence of any established treatments for COVID-19. World Health Organization (WHO) officials say at least 20 coronavirus vaccines are in development in the global race for finding a cure for the new virus.
Here, we look at some of the latest breakthroughs and significant studies that might help us fight against the ongoing coronavirus epidemic. We will know soon whether these developments will have any positive outcome.

A US biotech company has accelerated the production of an experimental drug that could become an effectual treatment for the novel coronavirus. According to Gilead Sciences (an American biotechnology company), the first clinical trial of the antiviral medicine remdesivir in COVID-19 patients is expected to disclose its findings in April. Remdesivir was originally developed to treat Ebola and is being considered a hopeful prospect for treating severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2).
“As a therapy, it could potentially help make people’s disease less severe, save lives for those hospitalized, and be used prophylactically for hospital workers and perhaps even in the community to limit spread out there,” said Timothy Sheahan, a virologist who has studied the drug at the University of North Carolina, Chapel Hill.
Currently, there are three ongoing COVID-19 clinical trials in China and the United States for remdesivir, which is being manufactured by Gilead. US doctors have treated patients with the drug under the Food and Drug Administration’s compassionate use policy and at least one patient has recovered. Furthermore, researchers from the Vanderbilt University and the University of North Carolina at Chapel Hill had shown in 2017 that remdesivir (then known as GS-5734) could inhibit replication of the coronaviruses that cause both severe acute respiratory syndrome (SARS) and Middle East respiratory syndrome (MERS) in human lung cells. Hopefully, the new experiments will be able to fight the SARS-CoV-2 as well.
2. The US has started the first human trial of a vaccine for the new coronavirus
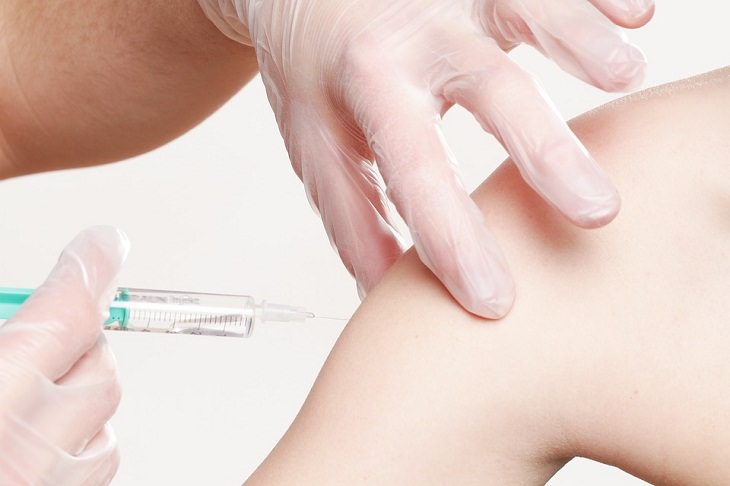
“When will we get a vaccine?” – this is the biggest question on everyone’s mind today. A vaccine, after all, is our biggest hope in stopping the novel coronavirus from spreading everywhere. The first major step towards this has been taken as the first human trial to evaluate a candidate vaccine against the new coronavirus has begun in the US.
The vaccine, called mRNA-1273, was developed by US National Institutes of Health (NIH) scientists and collaborators at biotechnology company Moderna. "The open-label trial will enroll 45 healthy adult volunteers ages 18 to 55 years over approximately 6 weeks," the NIH said. The first participant has received the investigational vaccine already. However, a commercially available vaccine could still be 12-18 months away.
The trial will study the impact of different doses delivered by intramuscular injection in the upper arm. Participants will be monitored for side-effects like soreness or fever. It is important to note here that coronaviruses are spherical in shape and have spikes protruding from their surface. The spikes of the virus bind to human cells and thus enables its entry into the body.
The Moderna candidate vaccine holds the genetic information of this spike in a substance that is called "messenger RNA." When the human tissue is injected with the spike's messenger RNA, it allows it to grow inside the body. Thus, it causes an immune response without having actually infected a person with the full-blown virus. A lot depends on this vaccine and its success will be detrimental to how we deal with the coronavirus pandemic.

Reports say that medical authorities in China have found a drug used in Japan to treat new strains of influenza to be effective in coronavirus patients. The influenza drug, favipiravir, has produced positive outcomes in clinical trials that were held in Wuhan and Shenzhen in China, involving 340 patients. The studies in China concluded that the drug was effective in treating coronavirus-related symptoms and had no clear side effects as of now.
In Shenzhen, the patients who were given the medicine turned negative after a median of four days after becoming positive. Furthermore, X-Rays showed an improvement in the lung condition of 91% of the patients who were treated with favipiravir, as opposed to 62% in those who were treated without the drug.
“It has a high degree of safety and is clearly effective in treatment,” said an official at China’s science and technology ministry to reporters.
In fact, China’s director of the National Center for Biotechnology Development has formally recommended the use of favipiravir as a way to treat patients diagnosed with the COVID-19. The influenza medicine was developed by Fujifilm Toyama Chemical and is also known as Avigan.
Doctors in Japan are also using the same drug for conducting clinical studies on coronavirus patients with mild to moderate symptoms. They are hoping that this will help in preventing the virus from multiplying in patients.
Israel’s Institute for Biological Research is expected to announce the development of a vaccine for the novel coronavirus soon. According to reports from the country, scientists have completed the development of a vaccine for the new coronavirus COVID-19. Apparently, they have achieved a crucial breakthrough in comprehending the biological mechanism and qualities of the virus. This includes the production of antibodies for those who already have the coronavirus and the development of a vaccine.
“Our basic concept was to develop the technology and not specifically a vaccine for this kind or that kind of virus,” said Dr. Chen Katz, MIGAL Galilee Research Institute’s biotechnology group leader. “The scientific framework for the vaccine is based on a new protein expression vector, which forms and secretes a chimeric soluble protein that delivers the viral antigen into mucosal tissues by self-activated endocytosis, causing the body to form antibodies against the virus.”
Endocytosis is a cellular process where substances are brought into a cell by surrounding the material with the cell membranes. This forms a vesicle containing the ingested material. After scientists sequenced the DNA of the novel coronavirus, they found that the poultry coronavirus has high genetic similarity to the human one and that it also uses the same infection system. This, according to the scientists at MIGAL, increases the chances of achieving an effective human vaccine shortly.
However, this process might take many months of clinical trials and experiments before it can be declared safe and effective.

A team of researchers from Canada’s McMaster University and the University of Toronto has successfully isolated severe SARS-CoV-2, the agent responsible for the ongoing outbreak of COVID-19. The team was able to culture the virus from two clinical specimens in a Level 3 containment facility.
Bear in mind that this doesn’t mean that people infected with the virus have been isolated. In simpler terms, it means that a pure sample of the virus has been obtained, which scientists have contained outside the human body for further study. “We need key tools to develop solutions to this pandemic. While the immediate response is crucial, longer-term solutions come from essential research into this novel virus,” said Dr. Samira Mubareka, microbiologist and infectious diseases physician at Sunnybrook.
According to experts, the isolated virus will help researchers all over the world develop better diagnostic testing, treatments, and vaccines for SARS-CoV-2, and also get a better understanding of its biology, evolution and clinical shedding. This will now hopefully lead to solving the COVID-19 epidemic.