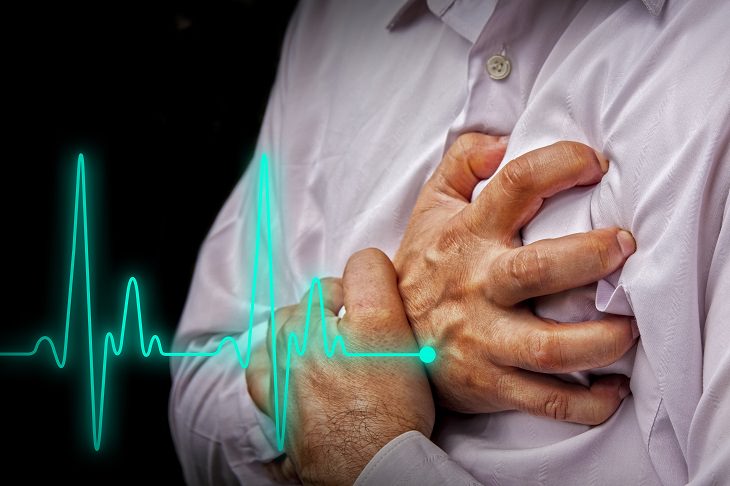
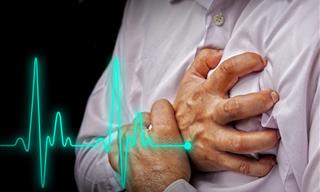
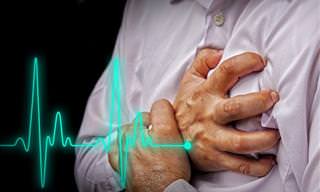
Symptoms of Tachycardia
• Accelerated heart rate (fast pulse)
• Chest pain
• Confusion
• Dizziness
• Hypotension
• Panting
• Sudden weakness
• Lightheadedness
• Palpitations – an uncomfortable racing feeling in the chest
Treatments for Tachycardia
Treatment options for this condition vary, depending on what has caused the condition, and the patient’s age and general health. The aim of the treatment is to tackle the cause of the tachycardia. When clinically applicable, the doctor may attempt to slow the rate, prevent subsequent episodes of tachycardia, and reduce risk complications. However, when no underlying cause is found, the doctors will have to try out different therapies.
Ways to Slow Down a Fast Heartbeat
Vagal Maneuvers
The vagal nerve helps to regulate our heartbeat. Maneuvers that affect this nerve include coughing, heaving, and placing an ice pack on your face.
Medication
Antiarrhythmic drugs that help to restore and control a normal heartbeat can be taken orally or by injection. Sometimes a patient might have to take more than one kind of antiarrhythmic drug.
Cardioversion
Paddles or patches are used to deliver electric shocks to the heart. This affects the electrical impulses in the heart and helps to restore a normal rhythm. This is done in a hospital.
Prevention of Episodes of Tachycardia
Radiofrequency Catheter Ablation
Catheters enter the heart via blood vessels. Then, electrodes at the ends of the catheters are heated to ablate (damage) the sections of the heart that are responsible for the abnormal heart rate.
Medications
When taken regularly, antiarrhythmic medications can help prevent tachycardia. However, patients may be required to take other medications as well, such as channel blockers, or example diltiazem (Cardizem) and verapamil (Calan), or beta-blockers, for example, propranolol (Inderal), and esmolol (Brevibloc).
Implantable Cardioverter Defibrillator (ICD)
This device, which constantly monitors the patient’s heartbeat, is surgically implanted into the chest. The ICD detects any heart abnormalities and delivers shocks to keep the heart rate normal.
Surgery
Sometimes, surgery is needed to remove a section of tissue. This procedure is only carried out when other therapies have been ineffective, or if the patient has another heart disorder.
Warfarin
This makes it harder for the blood to clot and it’s given to patients with a high or moderate risk of having a stroke or heart attack. Although this drug increases the risk of bleeding, it is prescribed to those whose risk of a stroke or heart attack far outweighs the risk of bleeding.
Causes of Tachycardia
• A reaction to certain medications
• Congenital (present at birth) electrical pathway abnormalities in the heart
• Consuming too much alcohol
• Consumption of cocaine and other recreational drugs
• Electrolyte imbalance
• Heart disease which has resulted in poor blood supply and damage to heart tissue, including heart valve disease, coronary artery disease, heart failure, heart muscle disease, infections, or tumors.
• Hypertension
• Hyperthyroidism (overactive thyroid gland)
• Smoking
• Certain lung diseases
Types of Tachycardia
Atrial Fibrillation
Sometimes, electrical activity can arise from the left atrium instead of the sinus node. This causes the chambers to contract at a high and irregular rate; this is atrial fibrillation. An episode of atrial fibrillation can last from a few hours to several days, and sometimes it may not go away until treated.
Atrial Flutter
The atria beat rapidly, but regularly. This condition is caused by a circuit problem within the right atrium. The contractions of the atria are weak because of the rapid heartbeat. An atrial flutter episode can last a few hours or a few days. It may also not go away until treatment is received. This is often caused by some form of heart disease.
Supraventricular Tachycardias (SVTs)
This refers to any tachycardic (accelerated) heart rhythm that originates above the ventricular tissue. The abnormal circuitry in the heart is usually congenital (present a birth) and creates a loop of overlapping electrical signals. An SVT episode can last from anywhere between a few seconds to a few hours.
Ventricular Tachycardia
Abnormal electrical signals in the ventricles result in a rapid heart rate. The speed of the heartbeat does not allow the ventricles to contract and fill properly, leading to poor blood supply to the body. This type of tachycardia is life-threatening and is usually treated as a medical emergency.
Ventricular Fibrillation
This occurs when the ventricles quiver in an ineffective way, resulting in poor blood supply to the body. If a normal heartbeat is not restored rapidly, blood circulation will cease, and the patient will die. Those with an underlying heart condition, or those who have been hit by lightning, may experience ventricular fibrillation.
Risk Factors for Tachycardia
• Age – people aged 60 and above have a much higher chance of experiencing tachycardia
• Anxiety
• Consuming large quantities of alcohol regularly
• Consuming large quantities of caffeine
• Genetics – people who have close relatives with tachycardia or other heart rhythm disorders have a higher chance of developing the condition
• Heart disease
• Hypertension (high blood pressure)
• Mental stress
• Smoking
• Using recreational drugs
Diagnosis of Tachycardia
A doctor can usually diagnose tachycardia by asking the patient some questions about their symptoms, carrying out a physical exam, and ordering some tests to be done. These may include:
Electrocardiogram
Electrodes are attached to the patient’s body to measure the electrical pulses that are given off by the heart. This test is also able to show any previous heart disease that may have contributed to the tachycardia.
Echocardiogram
This is a type of ultrasound investigation. By bouncing sounds of the structures in the body and registering the echoes, a moving image of the heart can be produced. This can help show structural or congenital abnormalities that might be playing a role in tachycardia.
Holter Monitor
The patient wears a portable device that records their heartbeat. It’s worn under the clothing and records information about the electrical activity of the heart while the person goes about their daily activities.
Blood Tests
This will help determine whether thyroid problems or other substances may be contributing to the patient’s tachycardia.
Tilt-Table Test
If the patient is experiencing fainting spells, lightheadedness, or dizziness, and neither the ECG or the Holter revealed any arrhythmias, a tilt-table test will be performed. This monitors the patient’s blood pressure, heart rhythm, and heart rate while they are moved from a lying to an upright position.
Chest X-Ray
This helps the doctor to check the state of the individual’s heart and lungs. Other conditions that could be causing the tachycardia might also be detected.
Possible Complications of Tachycardia
• Blood clots – these significantly increase the risk of a heart attack or stroke
• Heart failure – if the condition isn’t controlled, the heart is likely to get weaker. Heart failure is when the heart does not pump blood around the body efficiently or properly. The patients left, right, or even both sides can be affected.
• Fainting spells
• Sudden death – generally only linked to ventricular tachycardia or ventricular fibrillation.
Source: medicalnewstoday
Images: depositphotos
 Go to BabaMail
Go to BabaMail