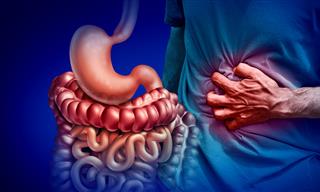
Understanding the gut connection
Doctors and patients have long suspected a connection between the gastrointestinal tract and Parkinson's. It was also noticed that constipation and other GI troubles are very common for a number of years before patients experience tremors and movement difficulty that lead to a Parkinson's diagnosis.
Dr. Allison Willis, a Parkinson's specialist at the University of Pennsylvania, who wasn't part of the study, but has many of her patients ask about the gut link says "This is a great piece of the puzzle. It is a fundamental clue."
James Beck, Parkinson's Foundation chief scientific officer, who too wasn't involved agreed that "there's a lot of tantalizing potential connections." Furthermore, he noted that despite its reputation, the appendix appears to play a role in immunity which may influence gut inflammation. In addition, the type of gut bacteria that live in the gut may also affect Parkinson's.
However, if it truly is common to harbor that Parkinson's-linked protein, "what we don't know is what starts it, what gets this whole ball rolling," Beck says.
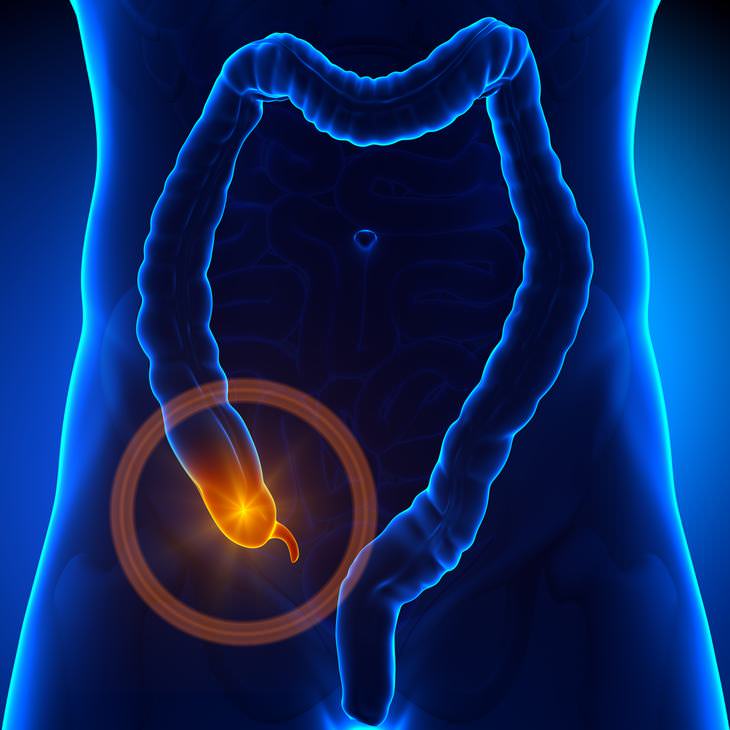
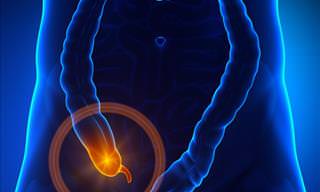
Scientists have for many years hypothesized about what might cause the gut-Parkinson's connection. One main theory included the possibility of bad "alpha-synuclein" protein which can travel from nerve fibers in the GI tract up the vagus nerve. This connects the body's major organs to the brain. Abnormal alpha-synuclein is toxic to brain cells involved with movement. There have also been other clues. Decades ago, people who have had their vagus nerve cut as part of a now-abandoned therapy had a reduced risk of Parkinson's. Smaller studies have suggested appendectomies, too, might be protective - but the results were conflicting.
Consequently, Labrie's team set out to find stronger evidence. Firstly, the researchers analyzed Sweden's national health database. They examined medical records of nearly 1.7 million people tracked since 1964. It was discovered that the risk of Parkinson's was 19% lower among those who had their appendix surgically removed decades earlier. What was found to be puzzling was that people living in rural areas appeared to get the benefit. Labrie said that it is possible that the appendix plays a role in environmental risk factors for Parkinson's, including pesticide exposure. In addition, further analysis suggested that people who developed Parkinson's despite an early-in-life appendectomy tended to have symptoms appear a few years later than similarly aged patients.
A common protein
Dr. Andrew Feigin, executive director of the Parkinson's Institute at NYU Langone Health, who wasn't involved in the research says that kind of study doesn't prove that removing the appendix is what reduces the risk. Consequently, Labrie's team examined tissue from 48 Parkinson's-free people. It was found that in 46 of them, the appendix harbored the abnormal Parkinson's-linked protein. So did some Parkinson's patients. Whether the appendix was inflamed or not also did not affect their findings.
This is a crucial finding because it means merely harboring the protein in the gut isn't enough to trigger Parkinson's, Labrie said. There has to be another step that makes it dangerous only for certain people. She says, "the difference we think is how you manage this pathology," she said, about how the body handles the buildup.
Her team plans additional studies. The findings are compelling, however, another key question is if the abnormal protein collects in healthy people's intestines. In addition, Penn Willis adds another caution: There are other unrelated risks for Parkinson's disease, this includes suffering a traumatic brain injury. "This could be one of many avenues that lead to Parkinson's disease, but it's a very exciting one," she said.
 Go to BabaMail
Go to BabaMail