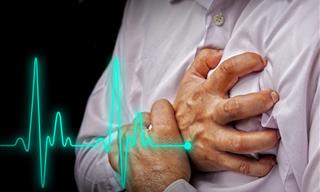
The common description of the sensation of a heart attack is that it feels like there is a heavy weight crushing your chest accompanied with a feeling of overwhelming anxiety. In films, you often see people clutch their chest, show extreme panic, and then collapse to the floor. It can happen like this, but not always!
A heart attack occurs when the supply of blood to the heart is blocked, usually by a blood clot. Despite the damage being caused in the body, some people experience no chest pain at all, which means that they do not seek immediate medical attention. Even those who get mild chest pain may just assume that it’s indigestion and only discover that they had a heart attack after an electrocardiogram shows damage to the heart. These are known as silent heart attacks, and a study that was published in 2016 found that this can occur in as many as 45% of heart attacks.
The important date for this research started being collected in the late 1990s and since then the diagnosis of heart attacks has improved dramatically, so the figure would probably not be as high as 45% today, but every year there are still people who, at the time, were oblivious to the fact that they were having a heart attack.
There are also patients who knew they were ill, but didn’t know what was causing it. They feel pain in their arms, neck, jaw or stomach and feel short of breath or lightheaded. They might start to sweat a lot or vomit. It’s the combination of symptoms rather than severe chest pains that allows for a diagnosis.
It’s often said that heart attacks without chest pain are more common in women, leading them to delay seeking help and reducing their chances of survival. In order to establish whether this is true, researchers in Canada in 2009 set out to measure the symptoms of a heart attack systematically, by studying 305 patients who were undergoing angioplasty. This is where a blocked vessel is re-opened by inflating a little ball inside it.
This surgery can often bring about the symptoms of a heart attack, so while the balloons were being inflated, the patients were asked to describe what they could feel. They found no differences between women and men in terms of chest or arm pain, shortness of breath, sweating or nausea, but women were more likely to have pain in the neck and jaw in addition to chest pain.
The findings from other similar studies have been pretty inconsistent, sometimes finding that men and women are equally likely to experience some chest pain, or that it’s more common in men. Sometimes the issue was clouded by researchers including other diagnoses alongside heart attacks in the same study. Therefore, in 2011, a review was conducted with the main aim of establishing whether there is a difference in the symptoms experienced by men and women.
Studies from Japan, Sweden, US, UK, Canada and Germany were all included, the largest having more than 900,000 participants. The data was taken from the best 26 of these studies, combined, and then re-analyzed. They concluded that women are less likely than men to get chest pain and are more likely to have symptoms such as nausea, fatigue, dizziness, fainting, and pain in the neck, jaw or arms. With both sexes, the majority still experienced chest pain, but a third of women and a quarter of men had heart attacks without any chest pains, making it harder for them to realize what was happening. If you don’t know you’re in a serious situation, you’re obviously less likely to call for help. On average, people wait two to five hours before seeking help.
A recent study has attempted to find out more about people’s thought processes in making what could turn out to be life-and-death decisions to go to the doctor. In-depth interviews with a small number of women who’d had heart attacks revealed that half knew something was up and went for help immediately. Three had vague symptoms which started off mild, but then got more intense, prompting them to visit the doctor. But the remaining people had absolutely no idea that their symptoms were to do with a heart attack and didn’t tell anyone else, deciding to wait and see instead.
Therefore, the lesson here is that a crushing chest pain is very serious and could indicate a possible heart attack, but so could a collection of other symptoms. Thus, we need to consider the possibility of a heart attack even when it doesn’t seem quite like it does in the movies.
Source: bbc
Images: https://depositphotos.com/home.html
 Go to BabaMail
Go to BabaMail