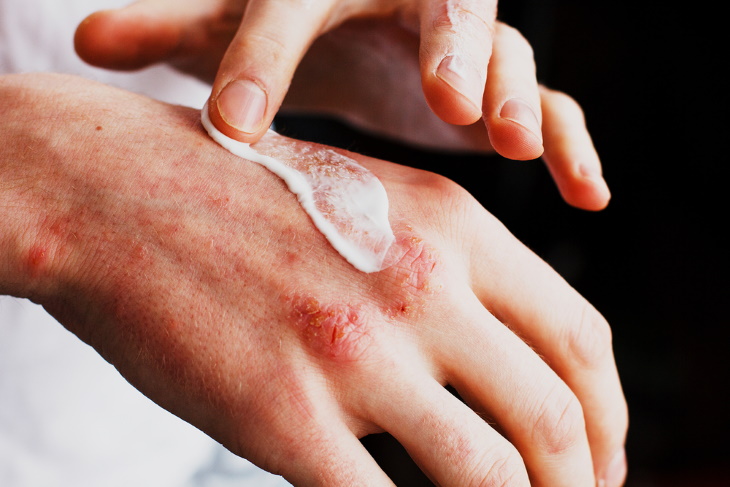
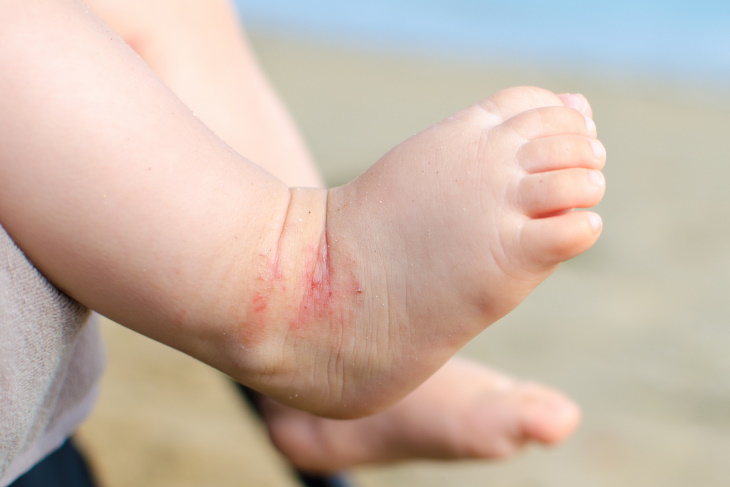
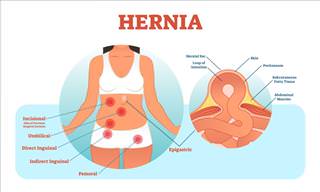
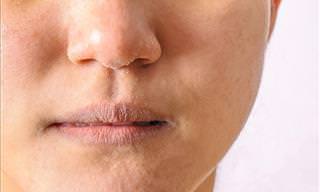
Winter is the season of snow, holiday cheer, and… dry skin. Indeed, the cold weather isn’t kind to the face and body, and for those who suffer from certain skin ailments, it’s also the time for annual flare-ups. This is the case with eczema, a skin condition that affects over 31 million people in the US.
In fact, eczema can manifest itself through itchy and dry skin or scalp, as evident by the alternative name of the condition, which is “the itch that rashes.” This uncomfortable condition isn’t as easy to treat as regular dry skin, so knowing how to tell the difference between these two conditions is crucial.
Dry skin and eczema – how are they different?
Eczema makes your skin itchy and flaky, so isn’t it the same as dry skin? This is a common question people have, especially in the winter when the dry and windy weather turns the skin red and itchy. While it’s certainly true that some forms of eczema (like contact- or seborrheic dermatitis) are more likely to appear in the winter, there’s a principal difference between the two.
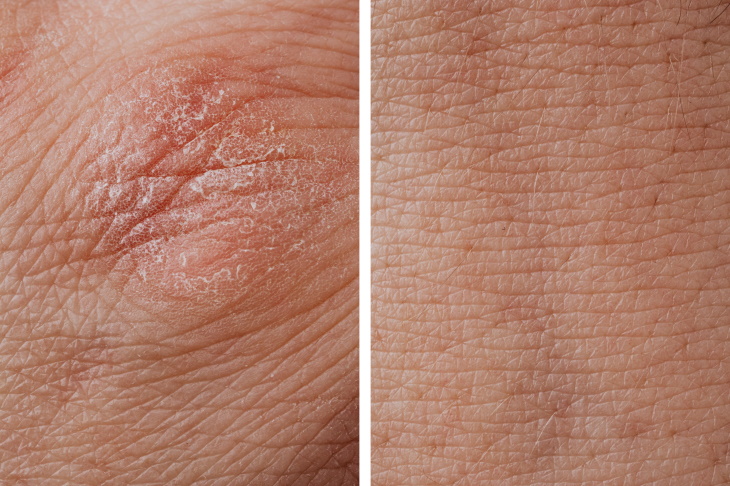
Dry skin is a skin type, whereas eczema is a chronic inflammatory skin condition. Even when eczema is triggered by an environmental cause, such as wearing woolen socks or taking a walk in cold weather, it won’t go away when we change the environment back to the baseline.
Unlike your itchy feet or dry hands that can be easily remedied by a layer of thick cream and a change of attire, an eczema flare-up will probably take longer to go away. The dry patches won’t always respond to moisturizing and may start developing thicker, darker, and itchier plaques.
If this pattern sounds familiar, and you experience some of the other symptoms we’ll mention, your “dry skin” may actually be an eczema flareup.
What is eczema?
Eczema is an inflammatory skin condition that causes one’s skin to become dry, bumpy, and extremely itchy. The name of the condition comes from the Greek word ekzein, meaning “to boil,” which alludes to the itching and burning sensations that often accompany the condition.
Individuals with eczema have a weakened skin barrier, which means that their skin is less effective at retaining moisture and protecting itself from germs and other environmental stressors.
In the past, it was thought that eczema was a condition that mainly affected children. Upon closer inspection, demographic studies reveal that anyone can develop eczema. In fact, the National Eczema Association reports that 10% of all people develop eczema in their lifetime.
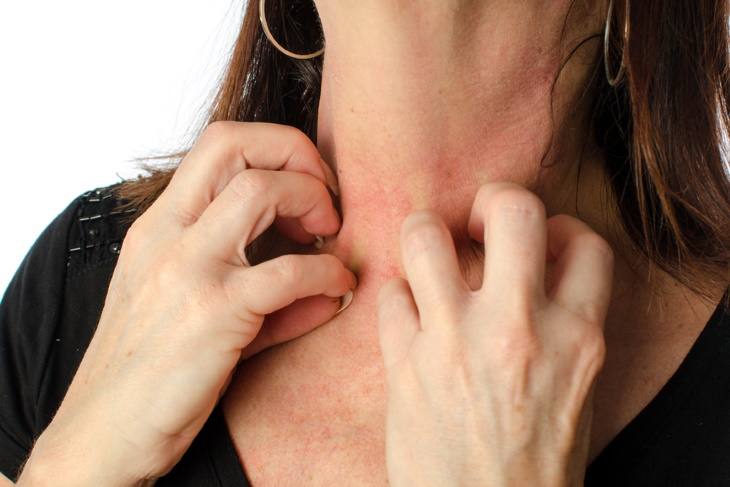
In a percentage of the population, eczema only appears later in life. Though the causes are difficult to pin down, medical experts suggest that it may have something to do with post-menopausal changes in older women, as well as the general tendency of skin becoming drier in late adulthood.
Eczema occurs in people of all skin tones, but it may look different depending on your skin tone. On pale skin, the rash usually appears in red patches. On medium or dark skin tones, it can take a darker brown hue or even look ashy or purplish.
General symptoms of eczema include
- Dryness
- Sensitive and inflamed skin
- Itchiness - eczema can be so itchy that people scratch the skin until it bleeds
- A rough, scaly, and raised rash
- Oozing or crusting bumps
- Hyperpigmentation.
Since eczema ranges from mild to severe, not every individual with eczema will experience all these symptoms.
Types of eczema
The terms eczema and atopic dermatitis are often used interchangeably, but the latter is merely one of seven different forms of this condition. Each type appears differently and comes with slightly different symptoms and treatments. Here’s a brief rundown of them all:
Atopic dermatitis (AD) is the most common form of eczema. It often begins in childhood and lessens or disappears by adulthood. AD manifests itself as a rash consisting of small itchy bumps filled with fluid. It often appears inside the elbows and behind the knees. Sometimes, AD turns into seborrheic or contact dermatitis in adulthood.
Neurodermatitis looks like AD. The patchy rash can appear anywhere on the body, scalp, and the back of the neck. Neurodermatitis is extremely itchy, to the point that people with this condition are known to scratch in their sleep until the skin starts bleeding and becomes infected.
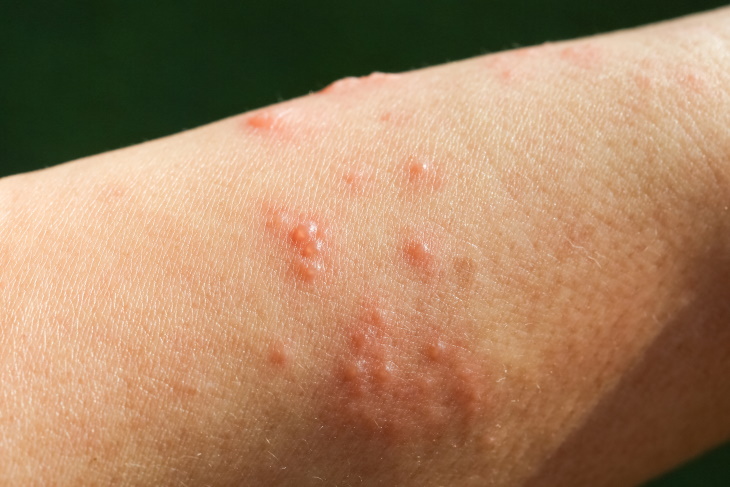
Contact dermatitis occurs when the skin gets in contact with an irritant, like bleach, nickel earrings, or latex gloves. The irritant causes itchy hives or pus-filled blisters to appear on the skin. Over time, the blisters heal, but the skin may remain leathery or scaly for some time.
Nummular eczema is easier to identify because it causes round, ring-shaped spots on the skin. It can be triggered by dry skin and insect bites, and it’s more common in people who already have another kind of eczema.
Seborrheic dermatitis causes dandruff or a rash to form in an area of the body with a lot of oil glands, like the scalp, eyebrows, or nose. Oftentimes, seborrhea is triggered by stress or hormonal changes in the body.

Stasis dermatitis occurs on the lower legs and the tops of the feet. It happens in people with blood flow issues and varicose veins, especially after a whole day of walking. When fluids ooze through weakened blood vessels in the skin, they cause an itchy rash to appear on the legs or feet. This type of eczema is more common in older adults.
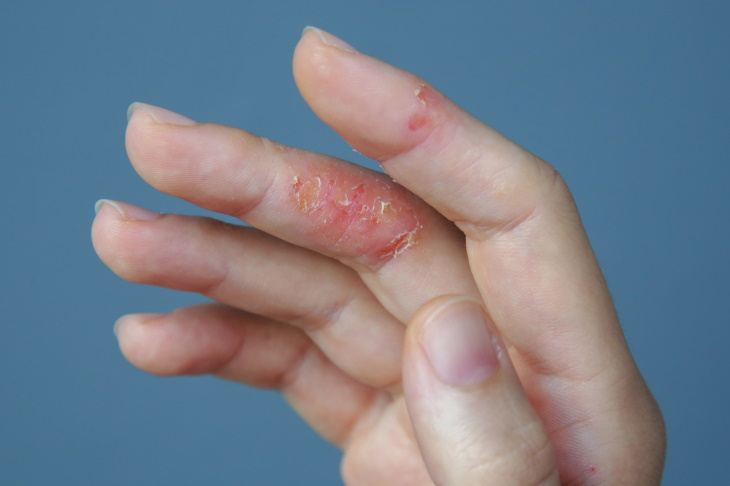
Dyshidrotic eczema is also known as hand eczema, although it can also appear on the soles of the feet. In patients with this condition, itchy and painful blisters form on the hands and feet, including between the fingers. Professionals who often get their hands wet and are frequently exposed to chemicals, such as hairdressers, are more likely to have this condition.
What causes eczema?
Eczema doesn’t have a single cause; it’s a complex condition that develops when several risk factors intersect.
First and foremost, the skin condition has a well-known link to allergies or asthma. Oftentimes, eczema flare-ups occur as an inflammatory immune reaction to a known allergen, such as dust, certain metals, fragrance, bleach, certain foods, etc. These allergic triggers are different for each person, so detecting your irritant does require a bit of detective work.
People who have asthma also have a significantly higher risk of eczema, which brings us to the second prominent factor in the development of eczema – genetics. To be brief, people who have family members with asthma, allergies, eczema, or dermatitis are more likely to suffer from eczema themselves. Scientists have also identified a specific genetic mutation that contributes to eczema. This mutation is linked to a protein known as filaggrin that weakens the skin’s ability to retain moisture.
Last but not least, one’s environment is also a factor. We often think that our environment plays a minor role in our physical health, but this is not the case with eczema. People who live in extreme climates, those who work with irritating chemicals and pollutants, those who wear and try a wide variety of beauty products, as well as those under massive stress are all more likely to suffer from eczema. That’s why you often need to consider your life holistically when addressing a chronic condition like eczema.
How is eczema treated?
Diagnosing the condition is the first step to success, and that is best done by a dermatologist, who will be able to tell it apart from similar-looking skin conditions like psoriasis or fungal skin infections.
Just like dry skin, most mild cases of eczema can be effectively treated at home. However, if you notice that the rash doesn’t go away on its own, you may need medicine to resolve the flare-up.
Below, we list several at-home treatments and remedies that work wonders for eczema:
References: National Eczema Association, American Academy of Dermatology, Mayo Clinic
 Go to BabaMail
Go to BabaMail