Parkinson’s Disease Explained
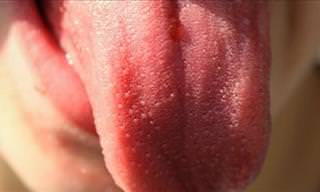
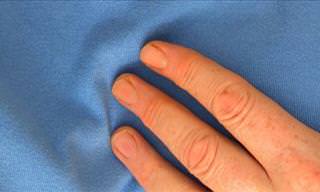
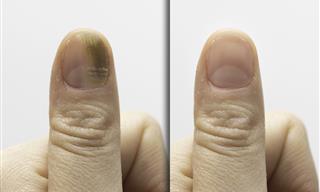
This disease is a movement disorder which gradually progresses. The disease typically begins around age 60 and symptoms include trembling, stiffness, slow movement and poor balance. Eventually, the disease progresses to difficulties with walking, talking and other routine activities of daily living. 50,000 people are diagnosed with Parkinson's in the United States each year. And while there is no cure available, treatment drugs such as levodopa, dopamine agonists and monoamine oxidase, among others have been found to help manage symptoms. Still, that are no known treatments that slow or stop the progression of Parkinson's disease.
Levodopa has been found to be the most potent and prominent drug used to treat Parkinson's disease. Though its effect tends to wear off over time. Negative side effects have also been attributed to this drug including dyskinesia (impairment of voluntary movement). This type of drug is usually reserved for people whose symptoms have become severe enough to interfere with activities of daily living and whose lifestyles are seriously compromised.
In people with advanced Parkinson's disease, when medications fail, deep brain stimulation (brain surgery) may also be considered to help alleviate symptoms.
For the most part, drugs are generally started at the lowest effective dose and treatment possible. But research supporting the advice: 'start low and go slow' is mixed. Peter Jenner, author of: 'Treatment of later stages of Parkinson's disease' says that "the introduction of L-Dopa (Levodopa) in those with longer disease duration or in high doses may result in a shortened period of good effect before motor complications appear. Very recently, keeping the dose of L-dopa below 400 mg per day in early PD was shown to reduce the risk of dyskinesia induction." However, he also goes on to note the following: "The early use of L-dopa was also shown to be the most effective treatment for motor symptoms and not to affect the long-term risk of dyskinesia."
New Drug Safinamide: How Does It Work?
People who suffer from Parkinson's disease, do not produce enough of the neurotransmitter, dopamine, in the brain. The cells that produce dopamine either die or, they may become impaired. But dopamine is necessary for proper motor control and movement. Furthermore, dopamine transmits signals in the brain that are involved in smooth, purposeful movements such as eating, typing and writing.
Adding to this, safinamide also modulates glutamate release. Though the specific effect of this action on the drug's therapeutic action is, as yet, unknown.
Safinamide is intended to be used in conjunction with other types of anti-Parkinson's drugs (such as levodopa) for later-stage disease.
When people first start treatment for Parkinson's symptoms, drugs generally work pretty well and symptoms can be controlled throughout the day. But as time progresses, usually between five to 10 years, the efficacy of conventional Parkinson's drugs wanes in many people, and symptom control becomes more difficult to alleviate. So, once levodopa stops working, it's hard to get people back to a stable baseline and a quality of life experienced earlier during the disease when levodopa and other drugs were working. Adding to this, even if motor difficulties are controlled, non-motor issues such as mood disorders, sleep disorders, and dementia become troublesome to those with later-stage Parkinson's disease.
Unfortunately, it cannot be predicted which people with later-stage Parkinson's disease will develop complications. Though it is believed that disease duration, disease stage, length of treatment with levodopa, doages, gender and body weight all play a role in eventual decompensation.

Understanding On Times and Off Times
'On Time': The periods when medications are working adequately and the symptoms of Parkinson's disease are controlled.'Off Time': The periods when medications wear off and symptoms, such as tremor, rigidity and difficulty walking reappear.
When safinamide is taken alongside of levodopa, the amount of On Time increases, while Off Time decreases.
The Clinical Trials of Safinamide
Two randomized clinical trials have shed light on the benefits of safinamide among people with more advanced Parkinson's disease. These participants had been diagnosed with Parkinson’s disease at either three or five years’ duration.
In the first clinical trial, 669 participants with motor fluctuations had been assessed. The participants either received sadinamide (alongside their other anti-parkinson's medication) or a placebo (alongside their other antiparkinson drugs). Results showed that the average ON time for participants varied between 9.3 to 9.5 hours.
After six months of testing, ON times increased in both sets of patients. But, it was seen that ON times were about 30 minutes longer in those taking safinamide. After two years of treatment, it was seen that average ON time stayed about the same in those taking safinamide, but decreased in those who were administered a placebo.
Aside from lengthening On Times and shortening Off Times, safinamide also improved movement (motor scores) in those taking it. Higher doses of safinamide also helped with activities of daily living and quality of life.
In a second trial, which involved 549 participants, an increase in On Time by about one hour was seen in those taking safinamide, as compared to those taking placebo. Off Time reductions were also noted. Furthermore, improvements in functioning and quality of life scores were also noted.
What are the Negative Side Effects of Safinamide?
Due to negative side effects of those taking safinamide, 3.7% of the participants dropped out of the study - in comparison to 2.4% of those taking the placebo. Common, adverse effects observed included:
• jerky or fragmented motions (i.e., dyskinesia)
• falls
• nausea
• insomnia
Less common but more serious side effects noted were:
• the worsening of high blood pressure
• visual hallucinations and psychotic behavior
• falling asleep during the day
• serotonin syndrome (when used with MAO inhibitors, antidepressants, and opioids)
• problems with impulse control or compulsive behavior (think OCD)
• fever and confusion
• retinal problems
The study also found that the following drugs should not be taken if you're also taking safinamide. The list includes:
• certain antidepressants (serotonin-norepinephrine reuptake inhibitors, tricyclics, and tetracyclics)
• cyclobenzaprine
• dextromorphan (found in certain cough medications)
• opioids
• St. John’s Wort
It was also found that although people with kidney impairment can take safinamide, those with severe liver problems should avoid the drug.

In Conclusion
It was therefore found that safinamide is most useful in those with mid-to-late stage Parkinson's disease who experience motor fluctuations. It was also noted that it will likely act better as an add-on therapy to primary treatment with levodopa and other antiparkinson drugs. Dyskenesia was observed to be the most common side effect. And, people with severe liver problems or those taking certain antidepressants and other medications should not take safinamide.
 Go to BabaMail
Go to BabaMail