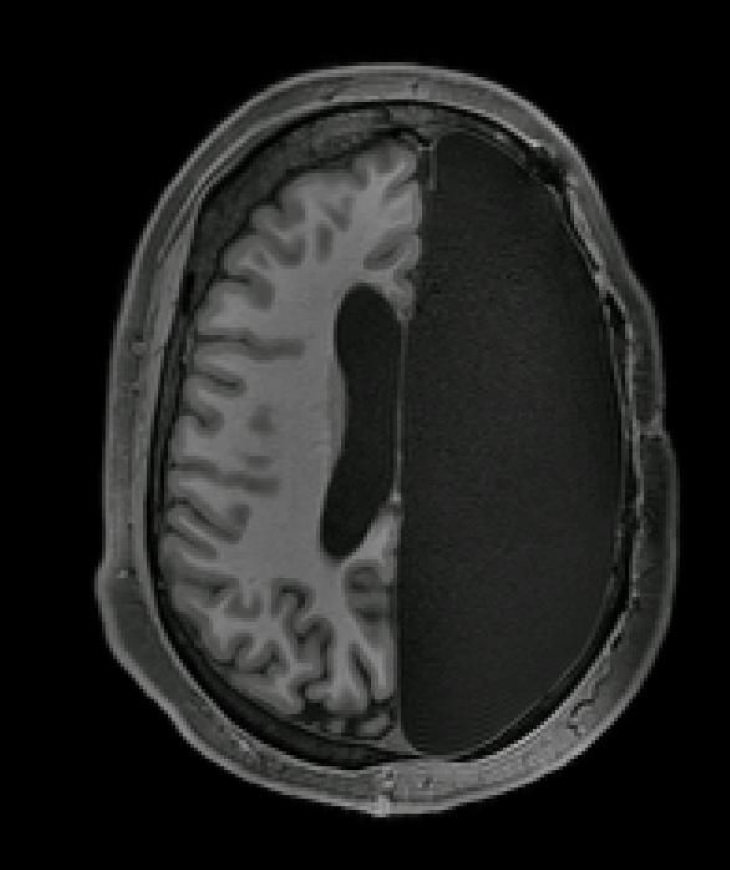
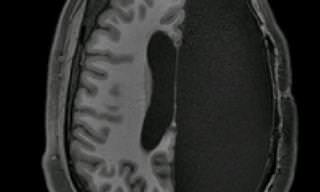
Our brain’s capacity to rewire itself and compensate for severe damage is something so astonishing it’s hard to comprehend. Probably the most evident examples of this amazing capacity are patients who have undergone a hemispherectomy - the surgical procedure of removing one of the brain hemispheres. Incredibly, these patients are often fully functional and you would probably never be able to tell they have half of their brain removed if you were to meet them.
Most often, hemispherectomy is conducted on kids, as before the age of three our brain is the most pliable and capable of rewiring itself. This is not to say that adults cannot get whole brain regions removed, however. As a matter of fact, resections, as these surgeries are called, are an effective method of treating medication-resistant epilepsy.
But let’s get back to hemispherectomies. How is it possible that the human brain can continue to function when as much as half of it is missing? Neuroscientists have long observed why that is the case, and the mechanism involved is something called neuroplasticity.
As you may or may not know, our brains are roughly divided into different regions, and most of these regions are responsible for doing a specific kind of task. For example, the part of our brain that’s responsible for vision is situated in the back of our brain and is called the occipital lobe (in green, see image below).
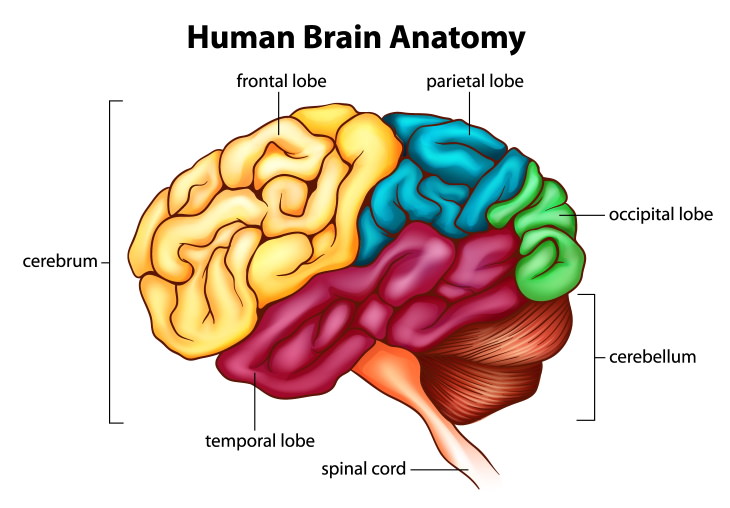
These divisions are very specific - certain brain regions are responsible for language, the movement of different body parts, psychological faculties and senses. But what happens when a brain region responsible for a certain function is damaged? Well, if everything goes according to plan, that function just gets moved to the nearest or comparable healthy brain region.
Furthermore, the younger you are, the more likely you are to fully recover, due to the fact that the ability of your brain to change decreases with age. This is exactly why hemispherectomy patients are typically children. Most often, these are kids suffering from epileptic seizures localized in only one brain hemisphere. In many cases, these patients are completely functional and live normal lives, "You can almost forget their condition when you meet them for the first time," said Dorit Kliemann, a researcher working with hemispherectomy patients in a recent interview.
But don't take our word for it, meet Jody, a young woman whose right hemisphere was removed at the age of 3.
Six hemispherectomy patients similar to Jody participated in a recent study at the California Institute of Technology, with the researchers trying to figure out how the brains of these patients managed to rewire themselves and how they function altogether. All six of the patients received the procedure to deal with epilepsy. The hemispheres affected by epilepsy have been removed in all of these patients at the age of 3 to 11 years, and they were in their 20’s and 30’s at the time of the study.
The researchers used the fMRI machine, a scanner that can show how the brain reacts to certain stimuli in action. When a certain brain region is more involved in a specific task, that brain region gets more blood flow, and the fMRI scanner shows that immediately.
The study revealed that the patients’ brains had much stronger connections than the brains of people with two hemispheres. Similar studies have also shown that brain functions that have two symmetrical centers in each hemisphere, such as vision, leg and arm movement, etc., tend to take the work for both sides in patients following hemispherectomy or resections.
In one study, for example, a boy regained vision in his left eye only two years following surgery that removed a third of his right hemisphere. These findings are absolutely incredible, but what’s more important, they can hopefully tell neuroscientists how the brain is capable of rewiring itself so that doctors would be able to treat brain injuries following strokes.
 Go to BabaMail
Go to BabaMail