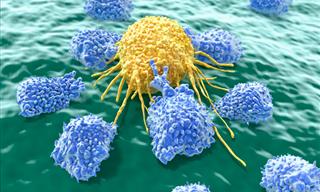
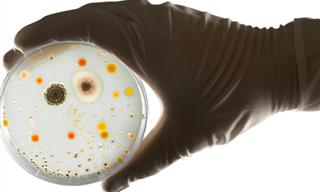
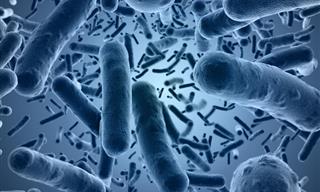
Infections caused by antibiotic-resistant bacteria pose a major threat to humans. Data shows that drug-resistant bacteria cause millions of deaths every year. The CDC says that more than 2.8 million antimicrobial-resistant infections occur in the U.S. each year, causing about 35,000 deaths. This growing health crisis may have just received a significant boost thanks to a group of scientists who claim to have developed a brand-new antibiotic that can destroy even drug-resistant bacteria.
Related: Will We Be Able to Solve the Antibiotic Resistance Crisis?
Scientists from Rockefeller University have synthesized a novel antibiotic using computer models of bacterial gene products. According to a study published in the journal Science, the drug, known as cilagicin, can kill even bacteria resistant to other antibiotics. It has been tested on mice, and employs a new mechanism to combat MRSA (a strain of antibiotic-resistant bacteria), Clostridium difficile (a type of bacterium that can cause severe diarrhea and colitis), and several other dangerous infections.
“This isn’t just a cool new molecule, it’s a validation of a novel approach to drug discovery,” says Sean F. Brady, the Evnin Professor and the corresponding author of the study, in a press release published by the institution. “This study is an example of computational biology, genetic sequencing, and synthetic chemistry coming together to unlock the secrets of bacterial evolution.”
A synthetic antibiotic can combat antibiotic-resistant bacteria
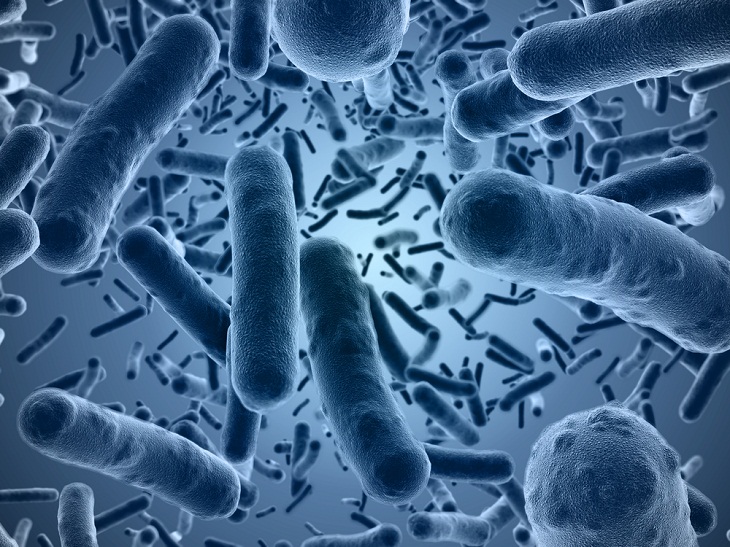
Since the beginning, bacteria have been inventing new methods to kill one another. Therefore, it’s not surprising that most antibiotics are based on bacteria. But bacteria's ability to evolve also results in the formation of antibiotic-resistant bacteria. And with the rise of these so-called superbugs, there’s also a growing need for new active compounds capable of eradicating them. Scientists estimate that countless antibiotics are likely hidden inside the genomes of stubborn bacteria that are tricky or almost impossible to examine in a lab.
Related: It’s Essential that We Debunk These Antibiotic Myths!
Brady and his team have been working on an alternative method for the past 15 years - finding antibacterial genes in soil and growing them inside more lab-friendly bacteria. But this approach has its drawbacks as well. The genetic sequences included in bacterial gene clusters are called “biosynthetic gene clusters,” which are groups of genes that work together to collectively code for several proteins. Unfortunately, with present technologies, such clusters are often hard to find.
Frustrated at not being able to unlock many bacterial gene clusters, Brady and his team took the help of algorithms. Modern algorithms can predict the structure of the antibiotic-like compounds that a bacterium with these sequences would produce. They do this by separating the genetic instructions within a DNA sequence. The team believes that organic chemists can then utilize the data and synthesize the predicted structure in the lab.
The prediction may not always be perfect, but the researchers feel they only need the synthetic molecule to be “close enough that it acts similarly to the compound that evolved in nature.”
Developing a new pool of antibiotics
Postdoctoral colleagues from the Brady lab, Zonggiang Wang and Bimal Koirala, began searching through a huge genetic-sequence database with the aim of finding potential bacterial genes believed to be involved in killing other bacteria and hadn’t been analyzed earlier. The “cil” gene cluster, which had not been examined in this context before, caught their eye because of its proximity to other genes used in the production of antibiotics. Next, the researchers began feeding its related sequences into an algorithm that proposed a few compounds that "cil" probably produces. They found that one compound, cilagicin, turned out to be a potent antibiotic.
The synthetic antibiotic cilagicin. (Credit: Rockefeller University)
Tests revealed that cilagicin killed gram-positive bacteria (germs with thick cell walls) in the lab and did not harm human cells. It even successfully treated bacterial infections in mice. Furthermore, the researchers found that cilagicin could combat several drug-resistant bacteria, along with bacteria grown specifically to resist the synthetic compound.
The team then confirmed that cilagicin works by binding two molecules, C55-P and C55-PP, both of which support bacterial cell walls. Bacteria often developed resistance to existing antibiotics by constructing a cell wall with the remaining molecule. Antibiotics like bacitracin bind one of those two molecules but never both. The team speculates that cilagicin’s ability to shut down both molecules may be an impregnable barrier that prevents resistance.
Related: Antibiotic Resistance - What's Being Done to Fight It?
Cilagicin hasn’t undergone human testing yet, but Brady and his team will continue carrying out further syntheses to improve the compound in future studies. They also intend to test it in animal models against more varied types of infections to confirm which diseases it may be most helpful in treating.
Share this post with friends and family
 Go to BabaMail
Go to BabaMail