Understanding Rheumatoid Arthritis (RA)

RA is an autoimmune condition that begins when the immune system mistakenly attacks its own healthy tissues. Apart from the joints, rheumatoid arthritis can damage other body parts, such as the heart, blood vessels, lungs, skin, and vision.
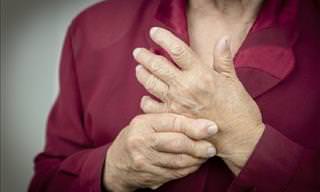
Symptoms of rheumatoid arthritis include:
- Joint stiffness, especially in the morning
- Tender and swollen joints that feel warm to the touch
- Firm bumps under the skin, commonly around the elbows.
The Centers for Disease Control and Prevention (CDC) suggest that mild symptoms of the disease usually appear around age 60 and gradually worsen over time, but RA can sometimes affect people in their 30s to 50s too.
Patients suffering from RA may also experience fatigue, loss of appetite, and fever years before the joint symptoms appear. That’s because the antibodies that damage the body’s own cells appear in the blood years before the onset of the first recognizable arthritis symptoms.
Learn more about Rheumatoid arthritis here - Do You Know the Basic Facts of Rheumatoid Arthritis?

This naturally makes us ask the question - what known factors contribute to the development of rheumatoid arthritis? For a while, we’ve known that genetics and lifestyle habits like smoking and diet play a role, but a growing body of research also suggests that intestinal dysbiosis, or an imbalance of gut microorganisms, may also be responsible for the appearance of RA.
More recently, scientists have managed to isolate a particular bacterium implicated in the development of rheumatoid arthritis - Prevotella copri.
What is Prevotella copri (P. copri)?
P. copri is generally considered a friendly gut bacterium that aids in the digestion of dietary fiber. The bacterium is even associated with improved glucose metabolism and a reduction in visceral fat (fat that develops between the internal organs). On the flip side, some scientists have linked P.copri to hypertension, insulin resistance, and chronic gut inflammation.
To that list of dangerous effects, a recent study published in Arthritis and Rheumatology has also added P. copri’s ability to trigger rheumatoid arthritis. The researchers found antibodies to P. copri in the blood sample of people with rheumatoid arthritis and those with an increased risk of the disease.
A study has found high levels of antibodies against a protein from a gut bacterium in people at risk of rheumatoid arthritis and those who already have the disease. A different study from 2019 that analyzed the gut bacteria species in people with RA also more Prevotella bacteria in samples taken from rheumatoid arthritis patients compared to controls. Lastly, an even earlier study specified that 75% of people recently diagnosed with rheumatoid arthritis had P. copri in the GI system contrasted with only 20% of healthy controls.
This evidence suggests that either the presence or an overgrowth of P. copri seems to contribute to the development of rheumatoid arthritis.
Gut Bacteria May Be Linked to Autoimmune Conditions
The authors believe that P. copri can travel from the gut into the bloodstream, where it triggers an inflammatory immune response. The bacterium may even be able to reach the joints and cause inflammation there.
The 2022 study we reviewed in depth examined specific antibodies in the blood that target P.copri. These two antibodies, called IgA and IgG, are known to provoke chronic inflammation. 98 patients with rheumatoid arthritis and 67 with an increased risk of rheumatoid arthritis, and an equal number of healthy control subjects were involved in the study. When compared to controls, the participants with rheumatoid had elevated levels of both antibodies, whereas those with a higher risk of RA had increased levels of just IgG.
These results suggest that P.corpi can cause inflammation in the joints or even contribute to the early onset of rheumatoid arthritis. In addition, these findings point to the fact that an overgrowth of gut microbiota may play a more significant role than anticipated in the development of autoimmune diseases in general.
That being said, the authors of the 2022 study recognize that P. copri may be the trigger behind only a subset of RA patients, as other gut bacteria and non-bacterial causes may also be able to increase inflammation and cause the condition.
Related article: A Few Simple Diet Changes That Can Prevent Inflammation
Can treating gut dysbiosis help rheumatoid arthritis?

An unhealthy diet and elevated stress levels are known to exacerbate the symptoms of rheumatoid arthritis. So, would the inverse be true as well? Could things like taking probiotics or maintaining a healthy diet reduce symptoms of RA or even reduce the risks of developing this condition?
There’s some emerging research that says ‘yes’! For example, a paper from 2020 found that maintaining a Mediterranean diet can reduce inflammation in patients with rheumatoid arthritis. According to the study, the participants also had a healthier gut microbiome, almost completely free of P. copri. Learn more about the Mediterranean diet here - I Began Eating Mediterranean After Reading This Advice!
In addition, probiotics can slow down the progression of RA and lower the risk of side effects in RA patients on immunosuppressant medication according to research. Last but not least, rheumatologists say that a combination of moderate exercise, not smoking, and a healthy diet can address gut dysbiosis and reduce the risk of RA.
H/T: Medical News Today
 Go to BabaMail
Go to BabaMail