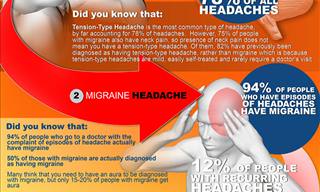
By: Dr. Arieh Kuritzky, Neurologist and Migraine specialist for over 40 years.
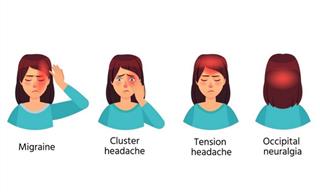
Headaches are one of the most common complaints doctors hear as about 80% of the population suffers from a headache at least once a year. Headaches can be divided into primary and secondary groups. Primary headaches have an unclear initial cause and can include migraines, stress-related headaches, cluster headaches, and even rarer types of headaches.
The secondary group includes headaches whose cause is known and effective treatment of it leads to its reduction. This group mainly includes sinus-related headaches, headaches stemming from the neck, headaches due to jaw joint injury, bleeding or an intracranial process, and headaches related to different parts of the face: eyes, teeth, muscles, and pulmonary nerves.

Migraines
Migraines are an ancient ailment and the origin of its name comes from the ancient Greek word HEMICRANIA meaning half head when translated into English and MIGRAINE in French.
A migraine is characterized by headaches that attack usually one side of the head, are pulsating in nature, last between 4 to 72 hours and are accompanied by nausea and/or vomiting or intolerance to light and noise. The diagnosis is clinical and is made by a doctor based on the patient's complaints. There are currently no tests to confirm diagnoses.
Since 1988 migraines have been diagnosed based on criteria set by the International Headache Society.
Criteria for diagnosing migraines:
1. At least 5 attacks
2. Headache attacks lasting between 4-72 hours (If not treated or treated without success).
3. At least two of the following four criteria:
- Unilateral location
- Pulsating quality
- Moderate to severe pain intensity
- Aggravation by or causing avoidance of routine physical activity (e.g., walking or climbing stairs)
4. During a headache at least one of the following two criteria:
- Nausea and/or vomiting
- Intolerance of light and noise
5. Not fit for any other diagnosis.

There are two main types of migraine:
1. Migraine without aura.
2. Migraine with aura.
Aura is a transient neurological disorder that typically appears before the headache phase. It lasts for 20-30 minutes and usually involves visual symptoms such as flashing lights, zigzag lines resembling forts (known as “fortification spectra”), or blind spots in your vision. Sometimes aura will manifest as tingling, pins-and-needles sensations in one arm or leg (paresthesias) or even difficulty in speech, or severe dizziness.
Migraine with aura accounts for 20% of migraines. About 2/3 of migraine sufferers experience migraine without aura and the rest suffer from aura on and off.
This type of headache can last for up to 3 days and is accompanied by symptoms which include nausea, vomiting, light and noise intolerance, sweating, diarrhea, pallor and, in extreme cases, confusion.
Recently, attempts were made to simplify doctors’ diagnoses by surveying many participants and finding common complaints, and a positive response to 2 of the 3 symptoms of nausea, light intolerance, and functional decline during the attack proved to be a good predictor of migraine attacks.
The quality of life of a person who suffers migraines with frequent attacks is difficult with migraines being defined as one of the most restrictive disorders. The disorder affects the patient's own health, family ties, social functioning, and ability to work and study. Quality of life is similar to that of someone who suffers from severe depression and lower than that of people who have suffered a heart attack, hypertension or diabetes.
Heredity
Migraines are possibly hereditary. If we go into a bit of detail - in a rare and specific form of migraine, the hereditary factor can be found in chromosome 19 which regulates the entry of calcium ions into the cell, part of the normal activity of the cell needed to function normally and transmit signals to other cells. The hereditary defect blocks the channels through which the calcium passes through, thereby disrupting the activity of the cell, but the problem is that in the common migraine the gene responsible has not yet been discovered.

Mechanism of migraine formation
Migraines appear to be a brain disorder rather than a vascular disorder as they were perceived until recent years. Aura is probably caused by a decrease in the functioning of a specific area of the cortex that progresses at a constant rate and is accompanied by a decrease in blood flow in these areas.
The changes in the cortex appear to affect the brain stem causing enlargement and inflammatory response in the blood vessels of the brain envelopes which is probably the source of the pain. The brain stem is responsible for the symptoms associated with migraine attacks such as nausea and vomiting.
Treatment
Treatment can be divided into pharmacological and non-drug treatments. Non-drug therapy focuses mainly on changes in lifestyle and avoidance of factors that induce migraine attacks. It seems that the brain of someone who suffers from migraines is affected by extreme conditions and therefore should be concerned with sleep and eating habits and avoid extremely stressful situations. In other words, migraine sufferers should avoid situations that put the body in an extreme state of hunger or fatigue or leave it in a stressful state.
Also, sufferers should avoid foods that trigger migraines, however, make sure that to identify which foods trigger migraines in each specific case as opposed to relying on general information found on the internet of possible migraine causing foods. The patient should keep track of their daily routine to learn what sets off their migraines. These factors change from time to time and are therefore frustrating, as they don’t help to regularly prevent headaches.
Drug therapy:
Drug therapy is divided into 2 main types:
A. Acute Treatment
B. Preventive Treatment.
Acute Treatment
Acute treatment can be divided into specific treatment mainly by special migraine medications called triptans and non-specific treatment by general painkillers such as aspirin, aspirin, etc. The specific treatment is only effective in migraines and doesn’t work against other types of pain, while non-specific drugs are directed against pain in general.
Triptans are a relatively new group of drugs that act on serotonin receptors. The receptors are located on the cerebral blood vessels, especially in the brain envelopes and nerve endings that affect these blood vessels. The action of the drug on the receptors prevents the expansion of blood vessels and the inflammation that is characteristic of a migraine attack.
Side effects include mainly weakness, a feeling of tension and discomfort in the chest, which are not related to the heart, are not dangerous, and usually pass quickly. The response to these drugs is very individual and cannot be predicted in advance, therefore it might be necessary to try several drugs until you find one that works for you. These drugs are safe and effective and often completely change the quality of life of patients. It has recently been shown that early administration of triptans results in a faster response to freedom from headaches and often reduces the chance of recurrence.
Preventative Treatment
Preventive therapy is designed to reduce the frequency, intensity, and duration of migraine attacks. This treatment should be implemented when there are at least 3-4 attacks per month that significantly limit daily functioning, and when acute treatment fails or is accompanied by serious side effects. Preventive drugs include hypertension drugs (beta blockers), antidepressants, anticonvulsants, calcium channel blockers, and anti-inflammatory drugs.
It is recommended to start with a low dose and to increase gradually. Also, you should wait at least 6-8 weeks to determine the effectiveness of the treatment and continue for at least 6 months. Sometimes acute treatment can be combined when an attack occurs while taking preventative medication. The choice of preventative treatment will be based on ancillary diseases, side effects, and contraindications. In women of childbearing age, birth control should be taken during treatment.
Drugs that have been proven effective in controlled trials are beta blockers (including PROPRANOLOL, METOPROLOL, NADOLOL) and others. People who have asthma, insulin-dependent diabetes, or have suffered heart failure should avoid this type of medication. In people who engage in competitive sports, these drugs may reduce physical fitness.
Recently, the use of anti-seizure drugs has been increased as a preventive treatment for migraines, with the two leading drugs being SODIUM VALPROATE (DEPALEPT) and, more recently, TOPIRAMATE (TOPAMAX). Their effectiveness is similar to that of beta blockers. Both drugs are well tolerated and used extensively. Depending on the underlying disease or condition, antidepressants, calcium blockers, or anti-inflammatory drugs may be added.

Chronic Daily Headache
Recently, there has been a growing body of evidence showing that in some cases migraines are an advanced disorder and may, therefore, shift from episodic attacks to chronic and daily. This change called “transformation migraines” involves in most cases (70%) overuse of acute medication but sometimes the transition is spontaneous and the cause is unclear.
Sometimes, migraines can begin as a daily frequency and the reason for this is also unclear.
It may be due to the formation of new patterns in the central nervous system. The threshold becomes minimal and the pain system is activated by external or internal stimuli which normally do not cause pain or a migraine attack. This information changes the considerations for preventive therapeutic intervention. Early intervention may prevent the progression of the disorder to the form of daily pain, the formation of irreversible changes in the brain and significant resistance to treatments of any kind.
The purpose of this guide is to share with you the ins and outs of migraines including the causes of migraine, the mechanism of its formation and various treatment methods. The conclusion that follows this information load is that the “migraines can’t be treated” era is over. On the contrary, medicine has a great deal to offer in the vast majority of cases. So if you suffer from migraines, see a doctor and get yourself take care of.
 Go to BabaMail
Go to BabaMail