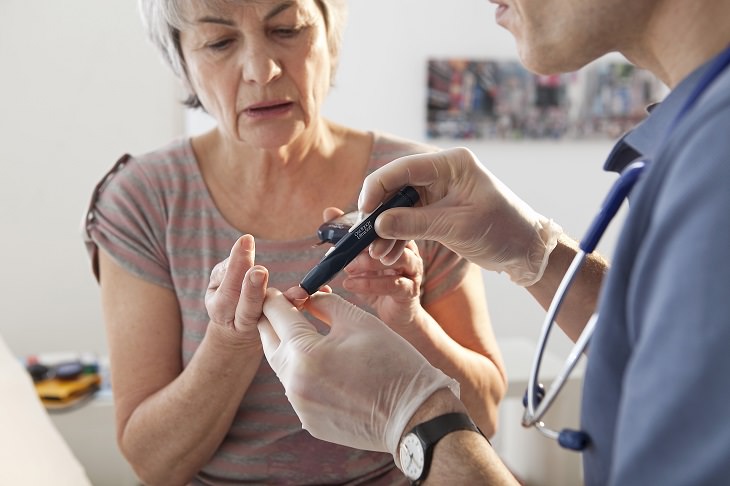
Therefore, it is definitely worth getting to know and keeping an eye out, for the symptoms of diabetes.
• You are above the age of 45
• You have already been diagnosed with pre-diabetes
• You are overweight or inactive
• You are African American, a native of Alaska, American Indian, Asian American, Hispanic/Latino, or Pacific Islander American, and are experiencing atypical symptoms.
Common Symptoms of Diabetes
If you’re experiencing any of the below, you should contact your doctor as soon as possible.
Excessive Urination (Polyuria)
Polyuria is an increase in the frequency of urination. When you have abnormally high levels of sugar in your blood, your kidneys draw in water from your tissues in order to dilute the sugar, so your body can expel it in the urine. The cells are also pumping water into the bloodstream to flush out the sugar, and the kidneys are not able to reabsorb this fluid during filtering, resulting in excessive urination.
To meet the clinical definition of polyuria, an adult’s urine output must be more than 2.5 liters per day (normal urine output is 1.5 liters).
As it’s near enough impossible for you to measure this yourself, if you notice that you’re visiting the bathroom more times than usual, consult your doctor.
Excessive Thirst (Polydipsia)
This usually goes hand-in-hand with excessive urination. As your body pulls water from tissues to dilute your blood and to dispose of the sugar through urination, the urge to drink increases. Many people describe this thirst as an unquenchable one. To stay hydrated, you drink excessive amounts of fluids – if these fluids contain simple sugars, your blood sugar levels will increase dramatically.
Extreme Fatigue
Your body is like a vehicle – it needs fuel to run. Its main source of fuel is glucose (sugar), which is gained from foods that contain carbohydrates that can be broken down. Insulin, a hormone created by the pancreas, takes sugar from your blood to your cells to use for energy. However, if you have diabetes, either your pancreas isn’t producing enough insulin or the insulin that your body is making isn’t being used properly, typically because the cells have become resistant to it. This ultimately results in your cells being deprived of sugar, or fuel. The result will be tiredness and extreme fatigue.
Cuts and Bruises That are Slow to Heal
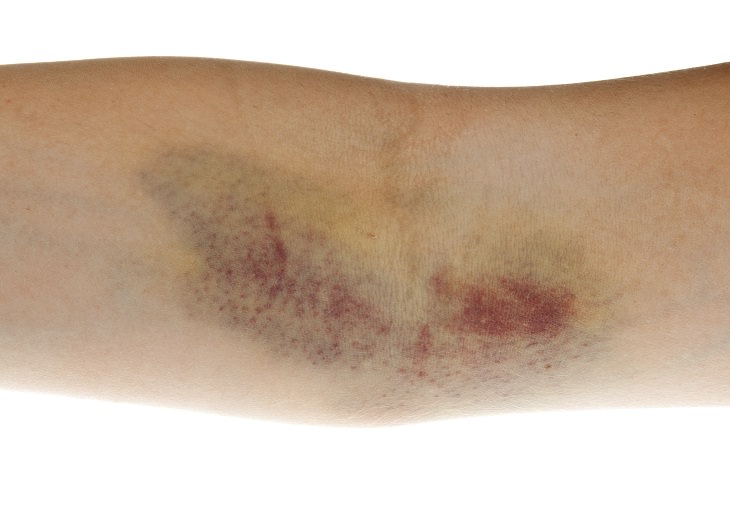
When the blood is full of sugar, nerves, and circulation can be affected. Adequate circulation is needed to heal as poor circulation makes it hard for blood to reach affected areas, slowing down the healing process. If you notice that you have a cut or bruise that is slow to disappear, this could be a sign of high blood sugars.
Excessive Hunger (Polyphasia)
This goes hand-in-hand with cell starvation and fatigue. As the cells are resistant to the body’s insulin, glucose remains in the blood. The cells are then unable to gain access to glucose, which will trigger hunger hormones to tell the brain that you’re hungry. Excessive eating can complicate things by causing blood sugars to increase.
Neuropathy
Numbness and tingling in the extremities is known as neuropathy. This is usually a symptom that occurs gradually over time as excess sugar damages the nerves. Keeping blood sugars within the normal range can help prevent further damage and reduce the symptoms.
Blurry Vision
Blurred vision can be a result of elevated blood sugar levels. Similarly, fluid that is pulled from the cells into the bloodstream to dilute the sugar can also be pulled from the lenses of your eyes. When the lens becomes dry, the eye cannot focus, resulting in blurry vision. Therefore, it’s important that all people diagnosed with type 2 diabetes have a dilated eye exam shortly after diagnosis.
Less Common Symptoms of Diabetes
The following symptoms are not experienced by everyone with diabetes, but they can signal the disease and are worth looking out for.
• Weight loss
• Erectile dysfunction
• Dry, itchy skin
• Frequent infections, such as yeast infections in women
• Irritability
• Dry mouth
How is Diabetes Diagnosed
The same tests used to screen and diagnose diabetes are used to detect individuals with pre-diabetes. There are a few ways you can be diagnosed. Your doctor can carry out a number of blood tests, depending on whether or not you have any symptoms. Whether you are at a high or low risk for diabetes, your physician will use the same tests:
• Random glucose test (if you’re symptomatic)
• Fasting glucose test (a test done when you haven’t eaten for 8 hours)
• Two-hour glucose tolerance test
• Hemoglobin a1c test (a three-month average of your blood sugar)
Sometimes people don’t experience symptoms of diabetes and the diagnosis is made not because the doctor suspects the disease but as a result of a routine check-up.
For someone who does not have any symptoms to be considered to have type 2 diabetes, they must:
• Have a fasting blood sugar (no food eaten for 8 hours) greater than or equal to 126 mg/dL
• Have a blood sugar of 200mg/dL after 2 hours during a glucose tolerance test using a 75g glucose solution.
• Have a hemoglobin A1c of 6.5% or higher.
If You’ve Recently Been Diagnosed with Diabetes
If you have just been diagnosed with diabetes, it’s normal to feel a bit scared, confused, and overwhelmed. There are so many myths floating about regarding diabetes, which can make it more difficult to cope with. Try not to listen to things that other people have to say, such as, you can never eat carbohydrates again. Instead, educate yourself.
Talk with your doctor about connecting with certified diabetes educators and receiving diabetes self—management education. Learning all about what to eat, what your medication does, and how to test your blood sugar levels are just some of the things these resources can help you with. Educators can also dispel myths, create meal plans for you, coordinate other doctor appointments for you, and listen to all your needs. They have been trained to teach using a patient-centered approach.

If You’ve Been Living with Diabetes for a While
We give you special kudos for managing your condition as it’s not always that simple. If you’ve had diabetes for a long time, it’s normal to feel burnt out sometimes. You may get tired of your day-to-day tasks, such as counting carbs or measuring your blood sugar. If this is the case, lean on a loved one for some support, or talk to someone else who has diabetes.
If you find that you’re a little bit rusty and could do with a refreshers course in nutrition or anything else diabetes-related, you should consider signing up for a diabetes conversation map class. These classes are a good way to re-learn the key components of diabetes in a group setting. If you have adequate knowledge and are looking for ways to make life easier, check out some apps, fitness trackers, or nutrition resources that can help you stay active and cook healthy meals. Keeping up this good work is worth it, as it can help prevent further complications.
If, on the other hand, you have started to develop complications or your medication regimen has changed because your blood sugar levels are getting higher, you should remember that diabetes is a progressive disease – and sometimes these things just happen without you being able to do anything about it. As you get older, beta cells in the pancreas tire and stop working. If you have had diabetes for 20 years and now need to start insulin, for example, it doesn’t mean that you have failed. It just means that your body needs some extra help. Make sure you continue to educate yourself, and that you continue to have someone to lean on when you need it, and keep communicating with your doctor. All this can truly make a world of difference!
Source: verywell
Check out our other guides on diabetes
 Go to BabaMail
Go to BabaMail