Restrictive Weight Loss Surgery
This kind of surgery involves shrinking the size of your stomach in order to slow down digestion. The average human stomach can hold the equivalent of three pints of food. Following restrictive weight loss surgery, this capacity immediately shrinks to as little as an ounce, later re-expanding slightly to two or three ounces. Due to this drastically-reduced stomach capacity, you’ll not be able to eat as much in a single sitting, and therefore the pounds will begin to drop off with ease.
Type 1: Laparoscopic adjustable gastric banding
During this procedure, a band containing an inflatable balloon is fixed in place around the upper part of the stomach. This is done to create a small pouch above the band, which results in a very small opening to the rest of the stomach. Next, a port is place under the skin of the abdomen. This is linked to the band via a tube, and is used so that fluid can be injected or removed as needed in order to adjust the size of the band. A gastric band is used for the purpose of ensuring that the patient feels full sooner when eating, however it does not reduce any calorie or nutrient absorption.
Advantages: A simpler and safer operation relative to the others on this list, minor scarring, fast recovery
Disadvantages: Less dramatic weight loss than with the other surgeries, possibility of lost weight being regained later on
Cost: $10,000-$33,000 (US prices, depending on state)
Covered by the Affordable Care Act: Yes (23/50 US states)
Mortality Rate: Negligible
Type 2: Sleeve gastrectomy
This procedure involves part of the patient’s stomach being separated and removed, with the remaining part being shaped into a tube-like structure. As detailed above, a reduced stomach capacity means that the patient can only hold smaller quantities of food following surgery. A secondary consequence of this surgery is reduced production of ghrelin in the body. Ghrelin is a hormone that regulates appetite. If less is being produced in the body, then the desire to eat is also reduced. Similarly to gastric banding, the body’s calorie and nutrient absorption are unaffected by this type of surgery.
Advantages: Ideal for very obese or sick patients, can be followed up with a gastric bypass if needed, nutrient absorption unaffected.
Disadvantages: Irreversible surgery, long-term benefits and risks still unknown due to the operation being a recent invention.
Cost: $9,600-$26,000 (US prices, depending on state)
Covered by the Affordable Care Act: Yes (23/50 US states)
Mortality Rate: 0.19%
Malabsorptive Weight Loss Surgery
In contrast to restrictive weight loss surgery, malabsorptive surgery is not concerned with shrinking a patient’s stomach capacity. Instead, it involves bypassing the small intestine, either wholly or in part. The idea behind this type of weight loss surgery is to reduce the body’s capacity for nutrient and calorie absorption.
Type 1: Roux-en-Y gastric bypass
This is the most common weight loss surgery performed today. In addition to being a malabsorptive surgery, it also adheres to restrictive principles. The patient’s stomach is divided in two, with the upper section of the stomach being sealed off from the lower. Next, the lower section is surgically connected to the small intestine. What this does is create a shortcut for food by allowing it to bypass the upper part of the stomach. By reducing stomach capacity, this also allows for fewer calories to be absorbed.
Advantages: Swift and dramatic weight loss, which results in highly positive effects on conditions such as diabetes, high blood pressure, high cholesterol, arthritis, sleep apnea, and heartburn. Weight also stays off for 10 years or more.
Disadvantages: Lowered nutrient absorption puts patients at risk of not getting enough nutrients, great care must be taken with diet, and dietary supplements must be taken daily by the patient until the end of his or her life. In addition, dumping syndrome, which involves food being dumped by the patient’s stomach into the intestines too rapidly prior to proper digestion, occurs in about 85% of gastric bypass patients. Dumping syndrome is often accompanied by bloating, pain, sweating, weakness and diarrhea. Last but not least, a gastric bypass is thought to be irreversible, however the surgery has been reversed in very rare cases.
Cost: $15,000-$57,000 (US prices, depending on state)
Covered by the Affordable Care Act: Yes (23/50 US states)
Mortality Rate: 0.2-0.5%
Type 2: Biliopancreatic Diversion/Duodenal Switch Biliopancreatic Diversion
A more drastic version of a gastric bypass, this procedure involves surgeons reducing a patient’s stomach size by as much as 70%. A biliopancreatic diversion incorporating a duodenal switch, in other words closing off the middle section of the small intestine and attaching the last section to the duodenum, is a less drastic version of the procedure. The duodenal switch is usually incorporated into the procedure should a prior medical decision be made to reduce stomach capacity by a lesser amount than in a full-blown biliopancreatic diversion.
Advantages: Even greater weight loss than gastric bypass, larger portion of the stomach remains following surgery in comparison to a gastric bypass or a gastric band. This means that the patient is likely to be able to eat larger meals than if he or she opted for the aforementioned surgeries instead.
Disadvantages: Much more serious risk of inadequate nutrient absorption than a gastric bypass, risk of dumping syndrome is just as high as with a gastric bypass.
Cost: $15,000-$25,000 (US prices, depending on state)
Covered by the Affordable Care Act: Yes (23/50 US states)
Mortality Rate: 0.1%
Electrical Implant Weight Loss Surgery
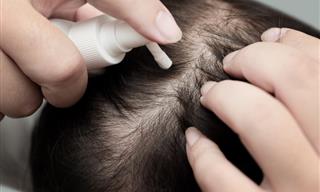
The most recently-devised type of weight loss surgery involves the implantation of an electrical device into your body, which interrupts nerve signals that are sent between the stomach and the brain.
Maestro Rechargeable Implant System
An implant, made by manufacturer Maestro, is implanted into the patient’s body. It works in a similar way to a pacemaker, delivering electrical pulses to a nerve that links the stomach and the brain. This nerve is known as the vagus nerve, and is responsible for telling the brain when the stomach is full. Seeing as the implant tricks the brain into thinking that the stomach is full, this reduces feelings of hunger.
Advantages: Least invasive weight loss surgery of all, procedure only takes an hour and 30 minutes.
Disadvantages: Implant has to be charged once or twice per week. A drained battery will require a visit to the doctor for it to be reprogrammed. Potential side effects of the latter can include nausea, vomiting, heartburn, belching and chest pain.
Cost: Minimum $15,000 per patient
Covered by the Affordable Care Act: Yes (23/50 states)
Mortality Rate: Negligible
 Go to BabaMail
Go to BabaMail