
A team of researchers from the university of Boston have reported their results to the New England Journal of Medicine, in which a new clinical trial successfully tested an artificial pancreas.
This test involved using a device implanted in type 1 diabetes patients that received both insulin and Glucagon (a hormone that elevates the blood sugar levels). To their delight, the device passed their expectations for its ability to automatically regulate blood sugar levels (preventing the 'sugar dump'), while also adjusting for both adults and teens, who require a larger amount of insulin.
"There is no treatment today capable of giving the results we've seen," says Dr. Edward Damiano of the University of Boston's Bio-Medical school of Engineering, and Head Researcher.
Protecting diabetes patients during the night
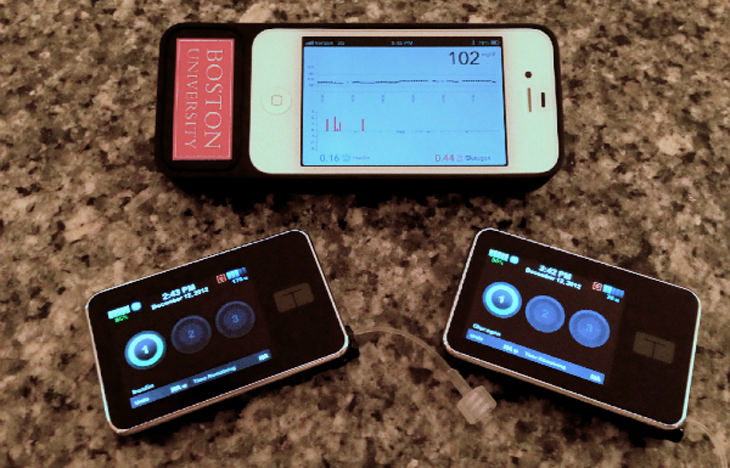
Ed has a personal stake in this. His 15-year-old son, David, has type 1 diabetes, and often his blood sugar drops in the middle of the night while sleeping, which can be deadly. This is why he and a colleague developed the 'bionic pancreas'. The device uses a sensor, an iPhone app and a special pump to deliver two materials: insulin, to lower blood sugar levels; and glucagon, which raises it. The pump, according to Damiano, works 24/7. "This is a relentless device, it doesn't take a vacation, it never goes to sleep," he adds.
Watch a video about the Bionic Pancreas' creation:
Protecting diabetes patients during the night
Ed has a personal stake in this. His 15-year-old son, David, has type 1 diabetes, and often has blood sugar drops, in the middle of the night while sleeping, which can be deadly. This is why he and a colleague developed the 'bionic pancreas'. The device uses a sensor, an iPhone app and a special pump to deliver one of two materials: Insulin, to lower the blood sugar levels, and glucagon, which raises it. The pump, according to Damiano, works 24/7. "This is a relentless device, it doesn't take a vacation, it never goes to sleep," he adds.
Ariana Koster has had type 1 diabetes since she was 11, and she is now getting outfitted for a bionic pancreas for the next phase of testing. "Just not having to worry about diabetes during the night is going to feel wonderful," she says.
Phase two of the test began yesterday and will take a year to complete. If all goes well, the device will be available to the public within 4 years. As for type II diabetes, the researchers believe it's definitely possible that it will help them as well, something they hope to look into during this year of testing.
Three parts
The bionic pancreas is made of three parts: two pumps, about cellphone size, that pump insulin and glucagon by need, and an iPhone wired to continuously monitor glucose levels. The components can be kept in a pocket or a fanny pack, and connect with three little needles that go under the skin, usually in the area of the belly.
The main advantage of the device, say the researchers, is its ability to free the patient from worrying about their disease all the time, and especially going to sleep without knowing if their blood sugar levels will drop to dangerous lows during the night.
Ariana Koster has had type 1 diabetes since she was 11, and she is now getting outfitted for a bionic pancreas for the next phase of testing. "Just not having to worry about diabetes during the night is going to feel wonderful," she says.
Phase two of the test began yesterday and will take a year to complete. If all goes well, the device will be available to the public within 4 years. As for type 2 diabetes, the researchers believe it's definitely possible that it will help them as well, something they hope to look into during this year of testing.
Three parts
The bionic pancreas is made of three parts: two pumps, about cellphone size, that pump insulin and glucagon by need, and an iPhone wired to continuously monitor glucose levels. The components can be kept in a pocket or a fanny-pack, and connect with three little needles that go under the skin, usually in the area of the belly.
The main advantage of the device, say the researchers, is its ability to free the patient from worrying about their disease all the time, and especially going to sleep without knowing if their blood sugar levels will drop to dangerous lows during the night.

The Musical Test That Could Detect Dementia Early
Researchers have developed a promising new approach: using music to detect the early signs of cognitive decline.

This Study Shows Where People Need to Be Touched
Touching is vital for human development in children, and it's also vital for the strength of familial and romantic relationships. Learn more here.

Breakthrough: Lion's Mane Mushrooms Boost Memory & Nerves!
Researchers have recently uncovered the mushroom's potent compounds, particularly hericene A, that could help nerve cells grow and better interact with each other.

Alcohol Linked To More Cancer Types Than Previously Known
A new study found a clear correlation between alcohol consumption and more types of cancer than previously known.
 6:14
6:14
What (Non-Psychedelic) Mushrooms Can Do for Your Brain
Lion's mane mushrooms are memory-enhancing brain food! Learn the science behind them here.

Study Finds a Painless Way to Monitor Blood Sugar Levels
A new study found that continuous glucose monitors improve blood sugar control and quality of life in diabetes patients - pain-free.

New Research Shows Eating Sweets Won't Make You Crave More
A groundbreaking new study challenges conventional wisdom, suggesting our preference for sweet tastes may be more stable than we think.
 5:17
5:17
How Exactly Do We Hear? All is Revealed Here!
In this informative TED-Ed video, Douglas L. Oliver explains the complete science behind hearing.

Chocolate Exposed! Here's What It Does to Your Brain!
Just what is it that makes chocolate so irresistible to so many people around the world? Find all of the answers in the article.

Enjoy This Fascinating Collection of NASA's Best Photos
Here are 15 of NASA's most amazing recent pictures, along with brief explanations of exactly what is going on in each one.
 5:14
5:14
Earth 2125: A Vision of the Future of Our Planet
Exploring what Earth could look like in 2125 reveals exciting potential.
 10:11
10:11
10 Smart Home Gadgets You Didn’t Know You Needed
If you’ve ever wanted a smarter, more efficient home, these 10 gadgets might be exactly what you need.

The 12 Game-Changing Inventions From 2024 You Missed
2024 was a ground-breaking year in terms of innovation. Here's a look at some of the key breakthroughs from the year.
 11:28
11:28
India Built a Monster Dam That Controls the Weather!
The Polavaram Dam doesn't just control floods - it moves water between regions and much more!

Science Lesson: 10 Fiery Facts About the Sun You Must Know
Learn some fascinating and little-known facts about the Sun in this article.
 4:26
4:26
Despite Looking Similar, Cats Are MORE Diverse Than Dogs!
Who's more diverse, cats or dogs? This video answers this question once and for all, the it might surprise you...
 10:30
10:30
China's Crazy Plan to Dig a Canal in the Middle of EUROPE
China is setting out a plan to dig a canal through the middle of Europe in the nearest future, but why?
 8:11
8:11
Fascinating: What is the Deepest Hole Humanity Has Dug?
This video explains how low humanity has dug down so far.
 18:14
18:14
Are These Vintage Kitchen Gadgets Any Good?
Will any of the vintage kitchen gadgets stand the test of time or outperform their contemporary alternatives?
 4:57
4:57
Fascinating: How Does Our Digestive System Work?
This video explains how the human digestive system does its daily.
 2:41
2:41
Trick-Mousing is Such Adorable Entertainment...
Mice are much cleverer than most people believe, and they easily respond to training, as long as you use positive reinforcement, or in other words - reward them frequently for their behavior with food.
 1:44
1:44
You Won't Believe What the Human Body Does in One Minute
How much do you think it is capable of doing in a single minute? Watch this video and you'll have your answer!
 17:03
17:03
What is a Ballistic Missile and is Its Purpose?
Why is the ballistic missile so feared, and what exactly qualifies it as such - will all be explained in this informative video.
 12:34
12:34
The World You See Doesn't Really Exist...
his video reveals how your brain constructs reality instead of simply perceiving it.

Explore the Most Bizarre Planets We've Discovered So Far
The search for stars, planets, and extraterrestrial life has led to quite a number of extraordinary discoveries, and here are 10 of the strangest!

These 14 Forgotten Robots Promised So Much...
This collection showcases 14 cool vintage robots that were supposed to change everything.
 36:24
36:24
Ever Wonder How a Steel Locomotor Works?
Let’s take a closer look at the engineering behind these compact workhorses.
 21:25
21:25
How Every Nuclear Power Got Its Atomics
This video will explain how each nation earned the complex and controversial title of nuclear power.
 3:02:59
3:02:59
Like Science Mysteries? Enjoy This Giant Compilation!
In this video, we unravel the greatest unsolved mysteries of physics.

Space Looks Breathtaking in These Amazing Photographs
There are some absolutely stunning photographs of space out there today, You won't believe how incredible it is!
 8:46
8:46
Science: What is Reality? Dive in and Find Out!
What if everything you see, feel, and experience isn’t real? The simulation argument suggests that our reality might be nothing more than an advanced computer program.

New Study: Dopamine Does Way More Than We Thought!
How the brain's reward system physically rewires the motor cortex during skill learning — and what happens when that reward signal gets cut off.
 8:12
8:12
The Tallest Statues Compared, Even Those Not Built Yet...
In this 3D animated size comparison, we showcase the tallest statues in the world alongside ambitious future projects.
 22:52
22:52
Will AI Take Your Jobs? An Expert Explains the Future
Gonzaga University's AI professor Graham Morehead some of our most pertinent questions related to AI.
 38:55
38:55
What Happens the Deeper You Go Underground?
What happens when pressure pushes matter beyond the limits of what we thought possible?
 20:04
20:04
Emotions Explained: The Science Behind How We Feel
Neuroscientist and psychologist Dr. Richard J. Davidson answers some fascinating questions about emotions you would never expect.
 42:14
42:14
Physicist Michio Kaku: The Universe in a Nutshell...
Physicist Michio Kaku explains the fundamental nature of our universe
 34:33
34:33
Is China Number 1 in Global Technology?
In this video, we’ll take a closer look at the new developments hitting the market — and what they could mean for the future of transportation.

7 Air Pollution Solutions That Will Help Us Breathe Easy
Let's take a look at some global initiatives that have been launched to reduce air pollution levels.

8 Important Inventions That Were a Complete Accident
It might be interesting for you to learn that some very important scientific innovations were born as a result of an accident.

There are Some Great Secrets Found in Mathematics...
Numbers hold some great secrets - they even tell us about life!
17 Incredible Eye Facts You Have To See To Believe
They say the eyes are the window to the soul, and they also happen to be our windows to the world. Here are 17 insanely fascinating facts about eyes.
 3:07
3:07
The Speed of Light Visualized in a Magnificent Video
Have you got the patience? Watch, in scale, just how long it takes light to travel from Earth to Mars
 6:25
6:25
Do You Like the Smell of Rain? This Is Why
One of the best things about rain and thunderstorms is that clean fresh smell afterward. But what actually causes that distinct scent?
These Are the Miracles That Happen in Our Bodies Every Day
There is a lot that happens inside our bodies every single day. Did you know any of these facts?

20 Useful Facts About the Science of Cooking
The science behind cooking is not often thought of, but it plays a crucial role in a dish turning out right. Here are 20 facts on the science of cooking.

10 Fascinating Facts About the Subconscious Mind
10 facts about the way the subconscious mind works
To enable your Ad-Free Subscription, please fill the fields below
Your subscription was successful, now you can enjoy an ad-free experience!! Note: To make sure you get no ads, please make sure to log in to your account. If you are logged in already, then refresh the page. The subscription can be cancelled at any time.


