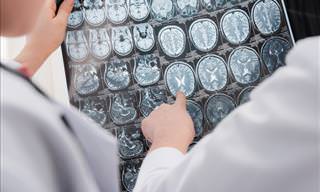
1. Depression
Depression is one of the most common and well-known mental health issues. Still, the condition is tragically underreported and underdiagnosed all across the world. Even in the US, a country where mental health awareness is rather high, only half of the people suffering from depression are diagnosed and connected with the right treatment. Depression is even more severely under-detected in developing countries.
The main problem with detecting depression is the fact that the condition can present itself in many different ways. For some, sadness and sleepiness are the main symptoms, but for others, depression manifests itself through headaches, cognitive decline, or even anger.

One social category that’s severely underdiagnosed with depression is the senior population. Oftentimes, depression can be confused for dementia or misrepresented as a side effect of chronic pain, cancer, or diabetes in older adults. According to Psychiatric Times, symptoms of depression can also coincide with symptoms of bereavement, namely, excessive guilt, worthlessness, visible slowing of physical and emotional reactions, and difficulty completing daily tasks. This is why depression is also often dismissed as grief.
It’s important to understand the full picture of depression and its many manifestations to get timely treatment for loved ones or yourself. To read more about the symptoms of depression, consider reading these resources:
- The 9 Signs of Hidden Depression
- Guide: How Best to Deal with a Loved One Going Through Depression.
2. Posttraumatic stress disorder (PTSD)
Posttraumatic stress disorder, or PTSD, is a mental condition that develops in response to an extremely traumatic life event. Disaster survivors, veterans of war, survivors of abuse or assault often manifest symptoms like social isolation, flashbacks, hypervigilance, insomnia, irritability, and loss of interest in daily activities.
These symptoms can be mistaken for other conditions, namely panic disorder, phobias, depression, alcohol abuse, and personality disorders. Scientists don’t know why people develop PTSD in response to traumatic events, but research shows that 20% of those who have been through some kind of trauma develop PTSD.
Oftentimes, the patients themselves are not aware of their condition, until a psychiatrist or therapist asks them about past trauma. “It is commonly missed especially when the client or patient doesn’t talk about the trauma of their past or if the psychiatrist or psychotherapist is not asking questions related to their past trauma. I believe PTSD is more common than it is diagnosed and might even be more common than depression, anxiety, and/or bipolar,” says Evanye Lawson, a licensed counselor.
Related Article: 6 Tips to Support a Loved One Suffering from PTSD
3. Eating disorders

Over 90% of people suffering from eating disorders are not medically diagnosed as underweight, which makes the condition extremely difficult to spot. In addition, eating disorders are often dismissed as something that only affects underweight teenage girls. In reality, eating disorders affect millions of people of every age, sex, and ethnicity, and they are especially rarely diagnosed in men and older people.
A study conducted by researchers at the University of Michigan School of Public Health points out, “Stereotypes about who develops eating disorders could contribute to disparities in diagnosis and treatment, with males, those of higher weight, people of color, and the non-affluent most likely to be slipping through the cracks.” All this is extremely alarming because eating disorders are the second deadliest mental illness - 10,200 Americans die because of an eating disorder every year.
4. Bipolar disorder
Bipolar disorder (BP) is one of the most serious mental health conditions. There is no cure for BP, but timely treatment can help patients manage their symptoms and prevent aggravation and complications. Patients with BP experience extreme shifts in mood and energy levels, jumping from states of apathy and depression to a state of mania or hypomania, when they feel overexcited or energized, often to a point that they engage in risky or dangerous behavior.
A survey by the National Depressive and Manic-Depressive Association concluded that 69% of patients with bipolar disorder are misdiagnosed. Of these patients, one-third are misdiagnosed for over 10 years. Most often, bipolar disorder is mistaken for depression. If the doctor fails to ask a depressed patient about manic symptoms, such as abrupt changes in mood, they will misdiagnose them. As Jamie Kreiter, a licensed clinical social worker, explained, “most people come in for treatment when they are depressed and so they meet the diagnostic criteria for depression.”
5. Substance-related issues
Alcoholism, drug use, and substance abuse, in general, are very heavy topics, and not only due to the stigma associated with them. We often think that a person who abuses alcohol, for example, is in control of his or her actions, that they choose to drink. This is not always the case. Yet, due to all the shame surrounding these issues, it easier for some people to hide their addiction than seek help. For this reason, many patients go undiagnosed for years, especially if they fit the mold of a stereotypical alcoholic or addict.
Age is one of the biggest obstacles in the diagnosis of substance-related mental illness. A 2012 report by the Institute of Medicine (IOM) suggested that 5-8million seniors have one or more mental or substance abuse conditions. The study also suggests that these numbers are estimated to increase to 10-14 million by 2030.
Research shows that these kinds of issues are much less likely to be diagnosed in older adults. This is likely due to the fact that the physical and cognitive symptoms of substance abuse often overlap with health conditions associated with aging. Malnutrition, dementia, cognitive decline, unexpected reactions to prescription drugs, and even stroke are all examples of symptoms that could be brought about by substance abuse.
Share this important information with others!
 Go to BabaMail
Go to BabaMail