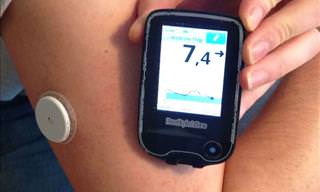
A class of medication that is commonly used to treat conditions such as incontinence, depression, and gastrointestinal disorders has been linked with an increased risk of getting dementia up to twenty years later.
In what is considered to be the largest study to date on the alleged link, researchers are encouraging doctors to seriously reconsider their options when it comes to choices of treatment.
The medical records of more than 300,000 individuals over the age of 65 were collected by an international team of researchers, a sample that includes close to 50,000 patients diagnosed with dementia. More than 27 million prescriptions for some form of anticholinergic medication were found among the records.
On analyzing these figures, the researchers found the proportion was skewed towards those with dementia, with 35% of those with the condition having been prescribed at least one anticholinergic fifteen to twenty years in the past.
In comparison, just 30% of those without dementia had a prescription. The numbers might seem close, but the difference is significant enough to warrant concern.
Noll L. Campbell, a pharmacologist from Purdue University in the U.S., says that, “anticholinergics, medications that block acetylcholine, a nervous system neurotransmitter, have previously been implicated as a potential cause of cognitive impairment.
The neurotransmitter plays a key role in the body’s neuromuscular communications, making it a choice target for a wide range of conditions that affect everything from fine motor skills to bladder control.
Having so many jobs to carry out means that a medication that beneficially interferes with one of the neurotransmitter’s tasks will no doubt have some undesired effect elsewhere. Doctors need to weigh these pros and cons when providing patients with prescriptions – having solid data like this will help them to make better choices in future.
Malaz Boustani, a medical scientist from Indiana University, says that “physicians should review all the anticholinergic medications – including over-the-counter drugs – that patients of all ages are taking and determine safe ways to take individuals off anticholinergic medications in the interest of preserving brain health.”
While being up-to-date on the research is a positive thing that can spark important conversations between doctors and their patients, it’s important to consider the evidence in context. This means not dropping your prescription.
Chris Fox, a clinical psychiatrist from the University of East Anglia, says that “further research is needed to understand possible reasons for this link. In the meantime, I strongly advise patients with any concerns to continue taking their medicines until they have consulted their doctor or pharmacist.”
Dementia is an increasing concern in our aging society, with diagnoses set to be more than double in countries such as the United States by 2050. In its mild form, it robs individuals of memory and at its worst, it contributes to an early death.
While headway is being made on ways to diagnose it earlier, limit risks, and even limit its impact, there is still much to learn about how the brain’s cognitive functions decline with age.
We cannot rewind the clock back a decade or two for those who are currently suffering from dementia, but with this type of evidence, it’s possible to strike the right balance in treatments to limit the risk for others.
Source: sciencealert
Images: depositphotos
 Go to BabaMail
Go to BabaMail